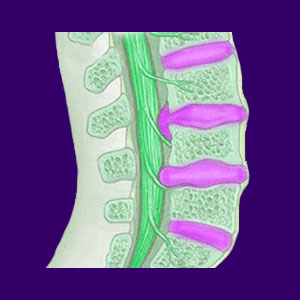
Thecal sac impingement is often noted on diagnostic imaging reports of people with various back pain and neck pain conditions. The thecal sac is the protective membrane which surrounds the spinal cord and other vital neurological structures. This membrane insulates and protects the nerve tissues, as well as holding cerebral spinal fluid, much like a reservoir.
There is plenty of extra space in this membrane and it is extremely common for central and paracentral herniated discs to be blamed for impinging on the thecal sac. However, in the vast majority of cases, this is absolutely no cause for alarm, since no neurological structures are affected.
This article provides some guidance for patients who are frightened by a diagnostic finding of thecal sac impingement, compression, displacement or effacement. We will help to clarify the diagnosis and provide the facts of its relevance to most chronic back, neck and sciatica pain conditions.
What is Thecal Sac Impingement?
Impingement is a term which means that something is pressing against the structure. In most cases, this is done by a bulging disc, although osteophytes and general osteoarthritic change can also impinge on the thecal sac. Picture a finger pushing into a water balloon and you will get the visual idea here. There are other diagnostic terms that are identical or similar in their meaning and these may include:
Herniated disc providing a mass effect on the thecal sac.
Herniated disc compressing the thecal sac.
Herniated disc encroaching on the thecal sac.
Herniated disc displacing the thecal sac.
In all cases, this means that the bulging portion of the disc is making contact to some degree with the thecal membrane and enacting some force against the side wall of the structure. This will produce a noticeable deformity which can be visualized on diagnostic imaging. However, this occurrence does not mean that any nerve tissue is inherently affected.
Let’s delve deeper into the relevance of thecal sac effacement diagnoses.
Thecal Sac Compression Concerns
In almost every case, impingement of the thecal sac is a complete nonissue. It is not symptomatic and will not cause pain or any related neurological effects. If the impingement is deep and reaches the spinal cord, or if a spinal nerve is possibly compressed, there may be the ideal circumstances for some symptoms to appear, but not necessarily. Luckily, when cord compression occurs, this can also be visualized using MRI and some other advanced diagnostic tests. If the cord is simply displaced, but not compressed, then symptoms may or may not be present, but the expressions should not be overly severe, if they even exist at all.
In some cases, in the lower lumbar spine, severe central canal stenosis enacted by a herniated disc or arthritic change may impinge on the thecal sac and actually compress one or more of the cauda equina nerve roots in the lateral recess or central canal. This event may explain why some people have sciatica even when the neuroforamen are clear at the affected level.
In these cases, the nerve compression may not be visualized, but can usually be correlated accurately by symptomatic expression. If the symptoms do not align to the suspected diagnosis, then the thecal sac compression is likely to be a circumstantial factor to the expression.
Thecal Sac Impingement Experiences
The thecal sac is one of those great back pain scapegoats and is often mistakenly targeted as a source of pain when touched by a herniation. The majority of diagnoses involving thecal sac encroachment are incorrect and horrific treatment results reflect this simple truth.
Remember that the thecal sac can be compressed without causing any injury in many cases, as long as no nerve structure gets caught up in the affected area. In fact, thecal sac impingement is so incredibly commonplace in the lumbar and cervical spinal regions.
In extreme situations, it is possible for patients with genetically narrow spinal canals to suffer other complications from severe herniations into the thecal membrane, including difficulty circulating cerebral spinal fluid. These circumstances apply to only a few cases I have ever seen, so do not worry unnecessarily.
Odds are if you have been diagnosed with thecal sac impingement due to a herniated disc, there is little, if anything, to worry about at all. I have a total of 12 known herniations in my spine. Many impinge on the thecal membrane and a few even displace the spinal cord. I have a very bad cervical herniation which bulges directly into my spinal cord in the lower neck and it is the most logical explanation for at least some of my diversified symptoms. It is very scary to see on the MRI film and even I do not like to look at it, since it can escalate the nocebo effect and set the stage for escalated symptoms due to fear alone.




