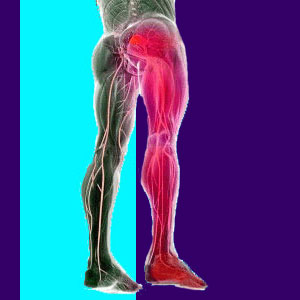
Piriformis syndrome is a lower body pain condition similar to sciatica in its expression, yet caused by a non-spinal source. True sciatica describes a condition where one or more of the spinal nerve roots are compressed or injured in the lumbar or lumbosacral regions, eliciting buttocks, leg, foot or toe symptoms due to neurological impairment. Meanwhile in piriformis diagnoses, the influence over the sciatic nerve happens lower in the anatomy and is brought on by suspected compression of the nerve by the piriformis muscle.
This muscle is deep inside the buttocks anatomy, under the gluteals. Usually, in a typical anatomy, the sciatic nerve passes directly under the piriformis muscle. In some people, the nerve actually passes through the muscle. Either way, the muscle is theorized to squeeze the sciatic nerve, causing it to suffer a compressive neuropathy condition.
This resource section provides a detailed look at the diagnosis of piriformis syndrome.
Piriformis Syndrome Diagnosis
This lower body pain syndrome is diagnosed most often by exclusion. If the patient has sciatic pain, but shows no spinal reason for a cause, piriformis pain syndrome is often pronounced as the working theory. A physical exam might create pain through motion of the hip, but this is common in many back pain conditions. Imaging on an x-ray or even an MRI will not typically show nerve compression, so the diagnosis is never 100%. Anesthetic injections are often used to confirm the diagnosis, but this method of symptomatic evaluation is not very accurate and might lead to a misdiagnosed pain condition in many patients. This is a very controversial condition which has been the topic of many medical debates among back pain specialists, but continues to generate treatment interest among care providers and patients alike.
Patients want an answer as to why they have pain. The piriformis provides a diagnosis and a plausible explanation for symptoms. Doctors find this to be an incredibly profitable condition to treat, since it involves long-term symptomatic relief using mostly hands-on modalities. The piriformis syndrome diagnosis makes both groups happy.
Piriformis Pain Topics
Piriformis pain syndromes are rarely immediately recognized for what they truly are. Most are misdiagnosed as traditional sciatica and it might take considerable time for an accurate diagnosis to be rendered.
The piriformis muscle used to be relatively unknown, but is now a villain in the medical community, due to its involvement in many lower body pain syndromes.
Piriformis exercises might help to bring about symptomatic relief, as well as boost overall health and physical conditioning.
Enjoying relief from piriformis pain can be possible using pharmaceutical treatment, holistic care methods or even minimally invasive surgical procedures or injection therapies.
Piriformis-Pain.Com is our niche web resource covering all manner of piriformis pain conditions, including piriformis syndrome, injury, degeneration and the common occurrence of sciatic nerve through muscle abnormalities.
Piriformis Syndrome Symptoms
This condition is most often described as feeling exactly like true spinally-induced sciatica. Pain in the buttocks and radiating down the backs or outer sides of the legs is the most common complaint. In addition to pain, the patient might experience tingling, numbness, burning or weakness in the buttocks, legs and/or feet.
Symptoms are often worsened by long periods of sitting, due to direct pressure exerted on the piriformis muscle and therefore, the sciatic nerve. Most piriformis patients do not have any actual pain in their backs, although some might suffer from related or coincidental structural or nonstructural issues.
Piriformis pain can mimic true sciatica in every way. Like sciatica, symptoms are usually long-lasting, often troubling patients for years. Learning how to cope with chronic piriformis pain requires expert guidance.
Piriformis Syndrome Treatment
Treatments for this condition are identical to conservative care for sciatica. Exercise, stretching, ice and heat are often employed. As always, these remedies do more to increase the circulation of blood to the area, than to treat the actual condition. If relief comes from these treatments, there is a good chance that the pain is due to oxygen deprivation rather than piriformis muscle problems.
Luckily, surgical intervention for piriformis issues is almost unheard of, sparing the patient from the barbarism which befalls so many others in the dorsopathy therapy sector. If there was a surgery which actually provided good results, it might be worthwhile. However, like in most back and neck pain issues treated with operations, cutting, burning and fusing does not seem to be the best route to a cure for almost anything… Statistically speaking, of course.
Learn all about the most common varieties of effectual piriformis treatment. Remember, piriformis therapy is typically nonsurgical in nature, so be cautious about acquiescing to any type of surgical intervention without considerable thought.
For more advice on attaining pain relief, please read our section detailing the full range of back pain treatments.
Piriformis Syndrome Conclusions
Many people who develop piriformis pain demonstrate the genetic abnormality in which the sciatic nerve passes through the actual piriformis muscle, rather than underneath it. This leads doctors to believe that the muscle is somehow responsible for constricting the sciatic nerve, eliciting symptoms. Most commonly, the theory behind why the piriformis affects the sciatic nerve is blamed on traumatic injury. However, ischemia makes far more sense, given the typical symptomology. Additionally, some patients with diagnosed piriformis pain do not even demonstrate the abnormality with the muscle surrounding the nerve. All in all, piriformis conditions are one of the more speculative of all common back pain conditions.
On a related note, I have studied piriformis pain in great detail in recent years and believe it to be a very real painful expression definitely related to muscular nerve compression, despite some doctors finding other explanations for the symptoms. My underlying causative process, however, differs greatly from the majority of doctors who make the diagnosis of piriformis syndrome.
I have heard so many care providers tell patients that they must have damaged the muscle to cause it to spasm so. Virtually all patients have no memory of this type of trauma and are often puzzled. A few doctors use the muscle imbalance explanation for piriformis spasms. Once again, the patient does not feel that there is any spasm occurring or any problem with the muscles in their legs.
I support the ischemia theory, based on evidence alone, and can understand why the process would affect the piriformis, especially in patients who demonstrate the structural irregularly of the nerve through the muscle. Dr. John Sarno wrote a logical explanation for this in his literary works when he details that the mind certainly knows of physical defects and abnormalities in the anatomy and often targets pain syndromes to fit these issues in order to make them more structurally convincing. Fascinating research material for those who are interested.
Piriformis syndrome responds incredibly well to our proprietary Cure Back Pain Forever Program. Best of all, the program is available anytime for immediate help for severe symptoms.




