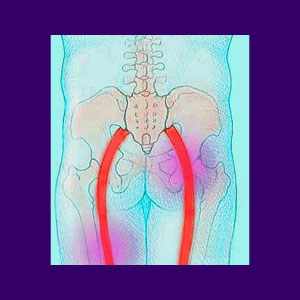
Piriformis therapy is a growing sector of care within the larger back pain industry. Piriformis syndrome describes pain being caused by sciatic nerve compression enacted by the piriformis muscle. This is a small but powerful muscle located under the gluteals in the pelvis. The piriformis rests on top of the sciatic nerve in most people, but sometimes, the nerve actually travels directly through the muscle in about 15% of the population. Symptoms seem to be found in greater numbers in people demonstrating this atypical nerve-through-muscle anatomy.
Piriformis syndrome is a diagnosis on the rise, despite being a truly controversial condition. It is also a diagnosis often made by exclusion, rather than by documented physical evidence. I find the theory to be quite enlightened in some respects, but lacking a clearly defined source process in most diagnosed cases.
This discussion centers on the use of various therapeutic modalities to target suspected instances of piriformis-generated sciatic nerve pain.
Reasons for Piriformis Therapy
If the patient is indeed suffering from piriformis-related pain, then there is no doubt that the use of some form of treatment might be appropriate. The correct choice of treatment is the main variable in this situation. Many modalities are really rather vague in their exact desired effects as a curative treatment.
Far too many common therapies are merely symptomatic treatments and do nothing at all to cure the underlying anatomical condition. The most common of these treatments are: drugs, injections, physical therapy and exercise. More drastic surgical measures for piriformis issues are definitely designed to correct the anatomical source of the discomfort, but often demonstrate poor statistical results for pain relief.
With piriformis symptoms, the patient is usually stuck between the choice of ongoing treatment to control the agony or a surgical correction hopefully leading to a cure. It is a tough choice to make and one that might have dire consequences either way, if the diagnosis turns out to be incorrect or even partially correct.
Problems with Piriformis Therapy
In piriformis syndrome, the pain is thought to be caused by muscular impingement of the sciatic nerve. Sometimes the sciatic nerve passes under the muscle and other times, it passes directly through it. Regardless, the patient has pain, with no other apparent cause, so the suspect is the piriformis muscle.
The diagnosis is often confirmed by injecting an anesthetic into the affected area. If the pain ceases, then the piriformis is usually targeted as the source of the symptoms. This is a poor diagnostic method since the anesthetic can spread and numb a larger region. The anesthetic will also relieve the pain due to other processes, since it may affect the actual sciatic nerve itself.
Most care providers are puzzled as to the actual causation of a spasming piriformis. Most speculate that the patient somehow injured themselves, even if they do not remember doing it. This seems far fetched, given the deep internal location of the muscle, its inherent strength and lack of correlation to any injurious events.
Doctors might get the rest of the equation right for a change if they considered ischemia as the underlying reason for the tight piriformis to begin with. Think about what happens when a muscle is oxygen deprived. It will spasm and tighten uncontrollably, like a charley horse.
Since the diagnosis is only partially correct, most treatments will provide temporary benefits by increasing blood circulation and oxygen supply to the region. However, symptoms will return because nothing has been done to combat the source process responsible for the oxygen limitation.
Piriformis Syndrome Therapy Tips
Some patients may have purely structurally-enacted symptoms which mirror the ideals of true piriformis syndrome. There may be a history of actual traumatic injury or a significant anatomical abnormality which is causing the pain to ensue. However, these cases seem to be the minority of diagnosed patients.
Most cases better fit the ischemic model of pain more logically, based on expression, treatment results and personal psychological factors.
Remember, a great number of oxygen deprivation syndromes are directly related to the mindbody processes and may be better treated using knowledge therapy and not ongoing symptomatic medical care.
I always recommend seeing a specialist when it comes to piriformis therapy. Demand to understand the specifics of the diagnosis completely before accepting the theory of why you are suffering. If what you are told does not make sense to you based on no history of injury, then be sure to research other possible causes for your pain, including ischemia. The more you know, the better your chances are of finding lasting relief from the misery.



