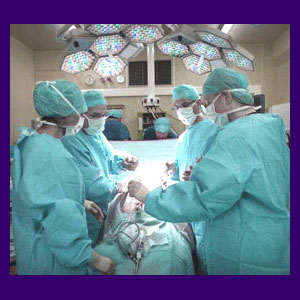
Surgery on the cervical spine is the second most common location for operations to occur in the human backbone. The cervical spine is an area commonly subjected to a full range of surgical techniques, since it is also the second most common area to experience pain, outdone only by the lower lumbar spine. The majority of symptoms and subsequent surgical undertakings in the cervical spine occur between C4 and T1, as these middle to lower vertebral levels normally demonstrate the most wear, as well as the greatest disposition towards injury in the neck.
Cervical spinal operations are always very significant treatments, so no procedure should be taken lightly. Even the least invasive type of surgery will inherently demonstrate serious risk factors which must be carefully considered and this is particularly true in an area that is as sensitive and vital as the human neck.
This discussion provides all the information that any pre-operative neck surgery patient needs to know ahead of their planned operation. If you are thinking about having neck surgery to cure your pain or resolve a functional deficit, then this article is ideally suited for your research needs.
Indications for Surgery on the Cervical Spine
Doctors will perform surgery on the cervical spine for virtually any reason and sometimes, for no specific reason at all, except to “treat” generalized neck pain that has not even been linked to a definitive source process. We find there to be few objectively justified reasons for performing neck surgery and countless reasons that are motivated by nothing more than soulless financial gain.
Some of the truly needed neck operations are performed to treat the following conditions:
Serious spinal instability, and especially macro-instability, must be treated surgically in order to ensure the preservation of neurological tissues and functionality.
Severe and verified versions of central spinal stenosis can create dire symptoms and will usually benefit from targeted surgical care.
Dire spinal curvature abnormalities, like extreme lordotic change, advanced cervical kyphosis (reversal of neck curvature and cervical, cervicothoracic or cervicothoracolumbar scoliosis may require surgical intervention in very rare cases.
Grade 3 and 4 cervical spondylolisthesis cases are candidates for surgical treatment when neurological tissues become threatened.
Times when surgery might be considered optional include treatment of the following conditions:
Verified foraminal stenosis leading to a pinched nerve may be easily treated using minimally surgical care.
Definitive osteophyte formation creating facet joint pain might benefit from minimally invasive surgical care.
Some cervical vertebral fractures might benefit from surgical fixation or repair.
Cases that virtually never warrant cervical spine surgery, yet are commonly treated using invasive care nevertheless, include all of the following very common scenarios:
Degenerative disc disease and herniated discs are almost never the source of chronic neck pain, but are blamed for creating symptomology more than any other type of spinal abnormality. It is therefore no wonder that disc-targeting operations feature the very worse curative results.
Minor scoliosis, lordotic changes, spondylolisthesis, spinal stenosis, foraminal stenosis and facet joint abnormalities that do not definitively demonstrate pathological activity should never be treated surgically. This includes over 95% of these conditions that are indeed treated surgically on a daily basis.
Surgical Cervical Spinal Procedural Options
Cervical spinal surgery can take many forms including any and all of the following procedural choices. All of these techniques are thoroughly detailed in our back surgery resource section:
Cervical discectomy and discotomy are the most frequently utilized techniques. Cervical IDET and nucleoplasty offer alternatives for treating some types of disc concerns.
Spinal disc replacement surgery is commonly used in the neck.
Laminectomy is one of the most versatile procedures, being used to treat a range of conditions that may cause spinal stenosis and neuroforaminal stenosis. Meanwhile, foraminotomy is used specifically to treat foraminal stenosis.
Nerve ablation and blocking techniques come in many forms and qualify as surgical symptomatic treatment for back and neck pain.
Kyphoplasty and vertebroplasty can repair fractures in the neck.
Spinal implants can be used to achieve a diversity of primary and secondary surgical objectives.
Corpectomy removes an entire vertebral body that has suffered irreparable injury or degeneration.
Spinal fusion is one of the most frequently used add-on surgeries in the neck, even though it has never been proven to provide a cure for any type of diagnosis or pain. Fusion is an extremely poor therapeutic choice and we have warned patients of its unnecessary application for over 18 years already.
Surgery on the Cervical Spine Considerations
If you do decide on neck surgery, then here are our best tips for successful outcomes:
Shop very carefully for your surgeon. Never simply accept the first doctor who provides a recommendation to undergo surgery. This person holds your life and future physical functionality in their hands. Choose wisely!
Minimally invasive techniques, including anterior procedures are ideal compared to fully open and dorsal approach operations.
Be sure to provide for all your postoperative needs well advance of having surgery.
Always implement knowledge therapy practices in addition to whatever surgical treatment you use to negate the considerable nocebo of the surgical process and optimize chances for a speedy and complete recovery.




