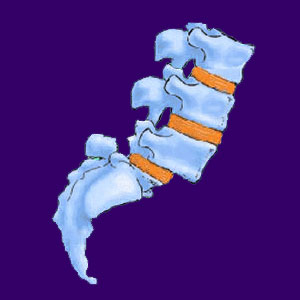
Spondylolisthesis is the medical term for front to back vertebral misalignment, also known as listhesis or vertebral slippage. There are many possible causes for vertebral misalignments to occur, ranging from congenital conditions, to back injury to normal spinal degeneration. Vertebral misalignment is further broken down into 2 distinct forms called retrolisthesis and anterolisthesis. These names detail the direction in which the vertebrae slip, either backwards or frontwards.
Spondylolisthesis is a condition that usually affects the L5 vertebra, but can actually occur almost anywhere in the spine in less common cases. The typical degenerative form usually starts with a stress fracture or other defect in the affected spinal bone. This defect is called spondylolysis. If the fracture is bad enough, the actual vertebra might shift forward and out of alignment with the rest of the spine. This is when a vertebral misalignment is pronounced.
This resource section is devoted to providing a comprehensive view of front to back vertebral misalignment abnormalities in the backbone.
Spondylolisthesis Experience
Many people have vertebral slippage and do not even know about it. This is especially true for congenital and early developmental cases in which the misalignment may have been there for decades prior to medical discovery. The vertebral migration is sometimes discovered by accident, when a person is undergoing an imaging study for a completely unrelated problem.
The majority of people with spinal misalignment conditions might suffer a significant nocebo effect upon diagnosis, particularly when their doctor really makes them worry about the long-term implications of the abnormality.
Spondylolisthesis can cause pain through several possible mechanisms. The first is pure mechanical back pain, which can occur when vertebral bodies do not move against one another properly and often suffer bone on bone contact. This will express itself in tightly defined areas and on particular ranges of motion. The most common form of symptomatic pattern is nerve pain, which can take place in more serious versions of vertebral misalignment. Remember, if the bones do not line up correctly, then the spinal canal and neuroforaminal spaces will not either. This can lead to central spinal stenosis or foraminal stenosis, also known as a pinched nerve.
Learn more about lower back pain which is enacted by lumbar vertebral misalignment.
Listhesis Topics
Vertebral shifting might be benign or may cause catastrophic effects in the spinal anatomy. No two cases of spondylolisthesis are identical. Therefore, it is best to learn everything about the condition before seeking medical care:
Spondylolysis is often a direct cause of vertebral misalignment.
Retrolisthesis describes a rearwards shift in vertebral position, while anterolisthesis describes a forward movement of a vertebral body, relative to other surrounding levels of the spine.
Slipped vertebrae usually exist singly, but some may occur in sequence, with more than one being shifted from typical positioning.
Listhesis pain and other neurological listhesis symptoms range from nonexistent to mild to moderate to severe or extreme, depending on many case-specific factors.
Spondylolisthesis treatment is a challenging proposition, with nonsurgical listhesis therapy being utilized to manage symptoms, while listhesis surgery might be prescribed to resolve the structural issues that cause pain.
Isthmic spondylolisthesis is the most often seen type of vertebral misalignment in the human vertebral column.
Are you affected by a vertebral migration problem in the neck or lower back? Spondylolisthesis-Pain.Com is the complete encyclopedia of spondylolisthesis, detailing the origins of the condition, its pain potential, the manner in which it is diagnosed and the best ways to treat the condition using conservative, moderate and invasive practices.
Degrees of Listhesis
The extent of the slippage is the most important diagnostic criteria, since spondy, as it is often called, is rated in 4 distinct categories:
Grade 1 is when the vertebra is out of alignment at less than 25%.
Grade 2 is when the vertebra is out of alignment between 26% and 50%.
Grade 3 is when the vertebra is out of alignment between 51% and 75%.
Grade 4 is when the vertebra is out of alignment between 76% and 100%+.
It is crucial to know that mild to moderate cases of spondy are quite common, especially in older adults who demonstrate significant lumbar degeneration. Most of these cases are not symptomatic, but should always be monitored by a qualified spinal specialist in order to make sure the condition does not deteriorate to a problematic degree.
Degenerative Spondylolisthesis
Osteoporosis can weaken the spinal bones and cause a fracture, leading to vertebral slippage. This is relatively common in older people and can affect multiple spinal levels. It is also possible for the condition to start due to a degenerative process. As we age, the spinal bones can get weaker and less stable. This process is usually due to arthritis in the spine. In this scenario, a vertebral bone slips forward and out of alignment with the rest of the spine. There is no fracture in this situation, just too much movement in the affected vertebra. This problem can lead to increased bone spur formation and spinal stenosis. This condition is really a combination of spondylolysis, disc degeneration and osteoarthritis.
Read more about degenerative spondylolysis.
Spondylolisthesis Guidance
Many minor (grade 1 or 2) cases of vertebral misalignment are not symptomatic, although they might take the blame for sourcing pain. If you have endured a broken vertebrae from trauma or a compression fracture, then this may be the possible underlying reason for your symptoms, instead of the vertebral slippage. The fractured vertebrae symptoms should go away by themselves, as the injury heals.
If you have chronic pain blamed on vertebral misalignment, consider your treatment options carefully. Conservative treatment is generally better for the condition and better for the general health of the patient. As always, be extremely careful when considering a surgical solution for any form of back pain. Make sure to consider the many back surgery risks of an operation before acquiescing to a surgical solution. Remember, the most common type of listhesis surgery involves a variation on spinal fusion, which is a drastic and often unsuccessful operation with a plethora of potential downfalls.
It should be noted that among all spinal irregularities studied, only spondylolisthesis creates a higher risk for the occurrence of back pain. This is most likely explained by the almost universally symptomatic conditions of grades 3 and 4 and is unlikely to provide a relevant comment on grade 1 and mild cases of grade 2.
Need help with severe spondylolisthesis symptoms? Our proven Cure Back Pain Forever Program address pain from 3 distinct perspectives, offering benefits for virtually all patients.




