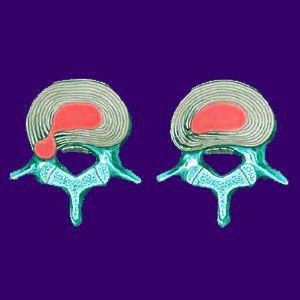
Herniated discs are extremely common spinal abnormalities that are often implicated in causing back, neck or sciatica pain. They occur when the thick outer layer, called the annulus fibrosus, has its symmetry compromised by internal pressure from the jelly center of the disc structure, called the nucleus pulposus. Herniations come in a great variety of types and severities, ranging from mild and completely normal bulges to cases where the structural integrity of the disc is completely lost.
Herniations are the most common of all structural issues in the spine blamed for sourcing pain, which is strange, since well documented and objective research clearly shows that most are complete nonissues. Studies show little, if any, correlation between the incidence of herniations and the occurrence of back pain anywhere in the spinal column.
This resource section provides an objective and complete view of intervertebral disc abnormalities. If you have been diagnosed with one or more herniated discs, then this is a discussion you need to read and understand.
Facts About Herniated Discs
It is worth mentioning for those who do not know that a spinal disc itself feels no pain. It has no internal blood supply or nerves and amounts to little more than a jelly cushion. The way that a disc can produce pain is to influence a neurological structure, such as a spinal nerve or the spinal cord.
Despite these facts, one thing is for sure: If you want to really inspire fear in anyone, tell them that they have a herniated intervertebral disc. The words alone are enough to bring some patients to tears and make others tremble to their very innermost core.
Herniated spinal discs are one of medicine’s great back pain scapegoats. They are found in a large percentage of the population, but only some people experience painful symptoms. Many people have one or more herniated disks in their backs and do not even know it. They do not have any pain. Read more about the obvious and less obvious causes of herniations. Understanding that most disc issues may have been there long before they are perceived to occur is vital for the recovery of affected patients.
Herniated Intervertebral Disc Topics
Intervertebral protrusions can be enigmatic to diagnosed patients. The fear factor is often a serious problem when a patient does not fully understand the extent of a disc problem that exists within their spine. We have taken much of the fear out of the equation by writing these objective essays based on proven facts:
Intervertebral herniation relief might not be needed, since many discs are not the actual cause of pain. However, for symptom-generating discs, finding lasting relief can be a tough proposition.
Disc herniation pain can only occur due to neurological compression or chemical irritation. Disc themselves do not feel pain. It is generally accepted that most herniated discs do not cause back pain even when they are symptomatic.
Disc herniation symptoms are certainly not limited to pain, but can also include various neurological expressions and functional deficits.
Diagnosis of herniations can be accomplished using advanced spinal imaging technologies, such as MRI or CT scan.
Herniated disc treatment is one of the most profitable and least effective specialties within the back and neck pain sectors of medical science.
Disc surgery can treat the symptoms of the herniation or the herniation itself.
Herniated disc surgery demonstrates poor statistical outcomes over timelines of 7 years or more.
Noninvasive intervertebral disc therapy might be the best course of action for many patients who choose to avoid an operation.
Herniated spinal disc cures are not common, but they can occur when the diagnosis is sound and treatment is delivered perfectly.
Disc herniation exercises offer a conservative fitness-based approach to coping with back or neck pain.
Disc herniation specialists can be physicians, chiropractors or therapists.
Looking to cure a disc problem? Be certain to read these disc herniation facts to get yourself on the correct path.
Disc herniations in the lower back, also typically called herniated lumbar discs, are the most common and numerous of all intervertebral abnormalities.
Disc herniations in the neck, also known as herniated cervical discs, account for many cases of intervertebral irregularity.
Never forget to consider the psychology of a disc herniation, since the condition is known to produce drastically negative mindbody effects.
Facts about spinal herniations tell the simple truth that medical science is headed in the wrong direction when it comes to diagnosis and treatment of many disc pathologies.
For detailed information on spinal disc problems, please visit our comprehensive herniated disc encyclopedia on The Cure Back Pain Network.
Types of Herniated Discs
A disc can bulge in several different possible ways. The way that it chooses to bulge will definitely play a major role in the scope and severity of symptoms it may create.
A disc will usually bulge posteriorly, inward towards the spinal cord.
It is possible for the disc to bulge towards the anterior, as well, but this is rare.
The disc can bulge directly in the middle, or more commonly, to one side or the other.
Nomenclature for Herniated Discs
The following are some of the many possible terminologies used to describe different types of herniations. This diversity of diagnostic terms can be incredibly confusing for any patient:
Bulging Disc
Slipped Disc
Collapsed Disc
Ruptured Disc
Extruded Disc
Prolapsed Disc
Disc Prolapse
Disc Protrusion
Add to this list the variety of descriptive and location-specific names used to detail herniated discs and you will really be totally lost! These terms include central, paracentral, median, medial, paramedian, paramedial, posterolateral, lateral, far lateral, foraminal, extraforaminal., focal, broad based, diffuse, sequestered and more.
The normal function of the intervertebral disc is to connect the individual vertebra in the spine, as well as act as a soft cushion in between the bones. It is like a natural shock absorber for the body. When this protective layer becomes damaged, there is a chance that the person might experience pain or other related symptoms. Discs also facilitate flexibility in the spinal column, creating the marvelous range of motion that we, as humans, enjoy.
Sometimes, a disc might develop an annular tear (a hole in the outer wall) and leak interior proteins from the nucleus. This process, called chemical radiculitis, is thought to produce nerve irritation is some patients, although the diagnosis remains controversial since most patients with known nucleus leakage are not affected by radicular irritation. It seems likely that only some people have particularly sensitized tissues to this specific protein, called tumor necrosis factor-alpha.
I know a lot about herniated intervertebral discs. I have 12 of them. My disc pain journey began with 2 known herniations at L4/L5 and L5/S1. With time, age and many injuries, I was diagnosed (at last count) with a total of 12 herniated discs, including every one from C2 down to T5. Lucky me. I try to keep it all in perspective and not let the nocebo effect take too heavy a toll on me. It can be hard sometimes, particularly since one very nasty looking disc is displacing my cervical spinal cord to such a great degree that the mental image of it makes me shudder. Not fun. This is not the only one touching the cord, but it is by far the worst looking.
Herniated discs respond better than any other diagnosis to our proven Cure Back Pain Forever Program. If you need immediate help, the program is available 24 hours a day from anywhere in the world.




