Sacroiliac pain is an often misunderstood symptomatic syndrome which can be blamed on soft tissue problems surrounding the joint, structural problems within the joint itself or a combination of the 2 terrifying circumstances.
SI joint pain is often described as being similar to sciatica in its usual expression. There is often radiating pain or weakness in the legs and buttocks, as well as general lower back pain. SI Joint pain is a diagnosis on the rise throughout the orthopedic community.
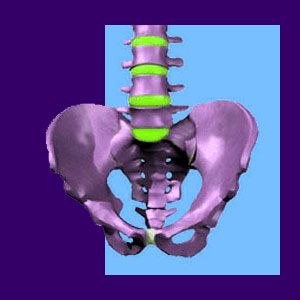
The sacroiliac joint is a small but incredibly strong joint that connects the sacrum to the pelvis. This joint acts as the main shock absorber between the torso and the legs. The SI joint is so durable that concentrated force applied to it will shatter the pelvis before the joint itself is damaged in any way. This makes it hard to believe that this bastion of fortitude might cause the type of agonizing symptoms often associated with the diagnosis.
It is not completely understood what exactly causes most SI joint pain conditions, which can be a sign of a potential psychoemotional causation or contribution in some patients.
Diagnosis of Sacroiliac Pain
The diagnosis of most cases of sacroiliac symptoms is made on the basis of exclusion. If there is no evidence of a lumbar spinal condition to blame for pain, then SI joint syndrome is often diagnosed, without or without supporting evidence. There are some tests to be done during examination, but they might elicit discomfort in any back pain condition, not just SI dysfunction.
An injection of anesthetic is often given into the SI joint under live x-ray, also known as fluoroscopy. If the pain goes away, then the SI joint is blamed. However, the anesthetic can affect virtually any regional nerve and might relieve pain not caused by sacroiliac issues. This is the unfortunate problem with conditions that are diagnosed by exclusion. We know what it is not, so therefore it must be…
Even when arthritic change is seen in the sacroiliac, there is usually no need for alarm. Remember that osteoarthritis is truly universal as we age and affects most or all of our major joints, leaving evidence which can be visualized on diagnostic studies. If OA were to blame for most SI pain conditions, then we would all be completely debilitated by the time we turned 50.
Painful Sacroiliac Topics
The sacroiliac region is very durable, yet is still a typical anatomical location for patient discomfort. The following studies each focus on a specific aspect of SI joint pain:
The sacroiliac joint is one of the strongest in the human anatomy, yet can still fall victim to injury, degeneration and various forms of dysfunction.
Sacroiliac joint injury can occur for many possible reasons and might be easy or difficult to treat successfully, depending on many variables.
Sacroiliac joint pain describes discomfort within the joint itself and possibly radiating into the surrounding areas of the buttocks, hip or leg.
SI joint sacroiliitis, also simply called sacroiliitis, describes structural changes within the SI joint that might be pathological.
Sacroiliac treatment spans the full range of options, including natural, medical and complementary medical care practices.
Sacroiliac therapy should begin conservatively and only progress towards invasive techniques as a last resort for severe pain.
Sacroiliac exercises offer hope for providing symptomatic minimization using constructive fitness practices.
Chronic sacroiliac pain is the unfortunate rule, rather than the exception. Statistics show that the majority of people with significant pain in the SI joint demonstrate chronic expressions for years of suffering.
Relief from sacroiliac discomfort should be relatively easy to find, as long as the underlying diagnosis is valid. Failure to find relief using indicated care often points to an inaccurate diagnostic conclusion.
Sacroiliac joint dysfunction describes pain brought on by soft-tissue problems, such as ligamentous laxity and tautness.
Sacroiliac-Joint-Pain.Org is the comprehensive resource for all sacroiliac joint pain issues. This website details the sacroiliac joint and all the possible pathologies that can create symptoms, as well as their respective causes. If you are not sure how to proceed with treatment, then this website will get you on the right path towards a cure.
Treatments for Sacroiliac Pain
Here are some of the most popular therapies used for diagnosed SI pain. Notice that they are all symptomatic in nature and will do basically nothing to resolve the supposed structural issues thought to be causative here.
Chiropractic uses manual adjustments to manage SI joint symptoms.
Physical therapy uses exercises and stretches to provide pain relief.
Pain management drugs bury agony under a pharmaceutical haze.
Back pain injections are long acting anesthetics used to dull SI discomfort.
Luckily, surgery is rarely necessary for SI joint concerns. More information on conservative therapies can be found on our page detailing back pain treatments.
Our proven Cure Back Pain Forever Program provides excellent results for sacroiliac pain. You can get immediate help 24 hours a day from anywhere in the world with our proprietary online program.
Guidance for Sacroiliac Joint Pain
Sacroiliac pain is a real enigma in my eyes. I see the facts of the anatomical structure involved and also observe how doctors will diagnose the basically normal and expected age-related changes found everywhere in the body to explain the symptoms.
How can such minor processes affect such a mighty piece of the anatomy? It makes little sense in most cases. Of course, there are times when the SI joint is truly horribly degenerated or affected by a significant soft tissue (ligament, tendon or muscle) issue in the area. These cases may require monitoring or even professional treatment. However, from my experience, these are the minority of cases and do not even begin to explain the huge number of diagnostic verdicts pronounced each and every year.
If you have tried to find relief using the usual methods and have not found any success, it may be time for a shift in your approach. There may be another reason why you are in pain. I highly recommend seeking some new diagnostic opinions from a variety of different types of doctors. Most of all, I recommend learning the facts of SI joint pain and looking for any holes in your own diagnostic theory by comparing your symptoms to the clinical expectations of the condition.




