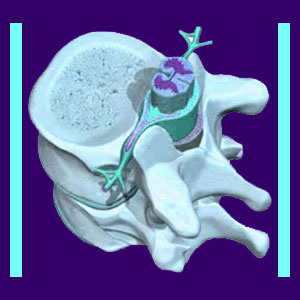
Laminectomy is a time-tested form of spinal surgery most typically used to correct pinched nerves due to structural impingement. This procedure is one invasive option for the treatment of spinal stenosis or spinal arthritis, but can also be utilized to treat herniated discs and various other spinal abnormalities when combined with other techniques, such as discectomy or foraminotomy.
Lamina removal procedures were traditionally generally performed as full open back surgery techniques and were very invasive. The incision would be up to 6 inches long and there would be complete dissection of all muscles in the affected area. Once the spine was visualized, part of the bone, called the lamina, was removed to reveal the nerve roots. The facet joints were trimmed to provide more room for the nerve roots to exit from the spine.
Now, minimally invasive forms of the technique are the rule, since fully open spinal surgery is barbaric, difficult to recover from and demonstrates far more risks. Endoscopic and laser versions of lamina removal can be just as effective and are less traumatic to the patient.
This patient guide provides a comprehensive overview of the lamina removal practices used to treat various spinal diagnoses.
Results of Lamina Removal Procedure
Symptomatic reduction is best achieved in patients suffering from sciatica in the legs. Actual back pain complaints enjoy less favorable results with this operation. As with any spinal surgery, the goal is to treat a specific structural issue. When this issue is indeed the source of pain, then treatment results will be good. However, being that this operation is geared towards suspected compressive neuropathy issues, which are the single most misdiagnosed condition in the dorsopathy sector, results are not always positive.
Patients recommended for lamina removal procedures are strongly advised to be sure their diagnosis is correct to avoid going through the trauma of this surgical nightmare for nothing.
Lamina removal is highly versatile and can be utilized in conjunction with many other surgical practices to resolve a wide range of problematic conditions that exist within the interior of the spinal structures and especially within the central spinal canal itself.
Recovery From Laminectomy
Patients are usually hospitalized for 2 to 3 days after surgery, although for minimally invasive versions the patient may be able to go home almost immediately. There is significant physical restriction due to the large incision in fully open versions. Most patients will have to restrain from most vigorous activity for 6 to 8 weeks post surgery. Patients will usually be prescribed physical therapy to help them recover from the procedure.
In order to increase your chances for positive results and a speedy recovery, it is crucial to get yourself in good shape and ideal health prior to the procedure and follow your doctor’s instructions for aftercare exactly. If a long recuperation period is advised, then patients must pre-plan time away from work and responsibility in order to commit themselves to getting better and nothing else.
Lamina removal practices are exceptions in the spinal surgery industry, since most recipients will not have to undergo more than one in a lifetime. This statistic is a refreshing change compared to commonly recurrent operations such as discectomy and spinal fusion.
Risks of Laminectomy Surgery
Lamina removal can always involve significant back surgery complications. This procedure is most often performed under general anesthetic and carries the usual risk of heart attack, embolism, blood clots or strokes. There is a chance of spinal fluid leak or nerve damage. There is a considerable risk for loss of spinal stability in the operated vertebral levels. A spinal fusion is sometimes performed at the same time, in order to prevent this occurrence. There is also considerable risk of infection, especially with such a large incision and multiple levels of tissue dissection.
The worst possible risk by far is the high incidence of failed back surgery syndrome. This occurrence is certainly every patient’s greatest fears come to life and can doom any patient to a lifetime of intractable pain that is unlikely to respond to subsequent care practices.
As previously mentioned, the most common reason why lamina removal will not help a patient is misdiagnosis of the theorized source of pain. Sure, a minor stenosis, disc or arthritic condition may exist, but these are clinically proven to have little, if any, correlation to the occurrence of symptoms. A great number of patients undergo surgery which is never needed, nor targeting the true underlying causation of pain.
Laminectomy Ordeal
My mother had the fully open version of this procedure in the late 1960’s, which left her with horrible scar tissue, limited mobility and pain that never did go away. She regretted the surgery and had a long recovery period to regain full functionality. I have also seen the results of this procedure in many other patients and I am not impressed. I would recommend that you investigate all possible options before even considering this invasive surgery.
Updated minimally invasive versions of this operation are now generally available and offer a much preferred path to treatment. The overall results are not much better, but at least the damage to healthy tissue is reduced and rehabilitation time is faster and less painful.
Laminectomy works best when used in combination with other surgical techniques and only when performed for strictly defined and indicated structural issues which have been definitively ruled to be the exclusive source of suffering. In all other cases, pursuing another procedure, or better yet, nonsurgical methods of care, might be preferred.




