A compressed nerve is a diagnosis often pronounced to explain obvious neurologically-based symptoms. Many physicians and chiropractors will have patients believing that nerve compression occurs constantly throughout the spine and causes a variety of painful expressions.
Although nerve compression does exist and can cause very serious health consequences, the condition is far less common than some healthcare practitioners would have us believe. Additionally some of the symptoms typically associated with a compressive neuralgia are not even usual parts of the actual diagnosis, including the common misconception of chronic pain.
This essay paints an accurate and vivid picture of the reality of pinched nerves in the spinal anatomy.
Compressed Nerve Reality
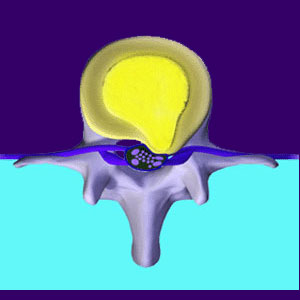
Nerve roots branch off the spinal cord through openings in between the vertebrae called neuroforamen. Injury and age can cause degenerative changes in the spinal bones, leading to a reduction in the spaces through which the nerves pass out of the spine.
Sometimes this space actually becomes too small for the nerve to pass without suffering from a pinching or squeezing effect from the spinal bones or discs. This is the reality of a pinched nerve condition. In order for the nerve to suffer true compression, it needs to be more than simply touched, contacted or displaced. It needs to have force exerted upon it, limiting or preventing it from functioning as expected in sending neurological messages.
Compressed Nerve Myths
The space required by a nerve to pass through the vertebral opening is very small. The opening would have to be almost completely closed off in order to effectively block normal nerve function. Although this is possible, it is simply not the anatomical case in the majority of patients diagnosed with pinched nerve conditions.
This is especially true when a herniated disc is the suspected culprit causing the nerve compression. Vertebral bones are hard and unyielding, but disc material is softer and more pliable. It is rare for a herniated disc to compress a nerve, unless the condition has time to age and calcify, creating a solid structure more capable of affecting nerve signal.
Scientific evidence demonstrates that continued compression of a nerve causes the nerve to lose the ability to signal altogether. The result of this situation is numbness, as well as possible loss of mobility and/or anatomical function.
Most patients with long-term nerve-related symptoms do not understand that pain is only a short term effect of common compressive neuropathy. This is information which needs to be recognized in order to find the solution to idiopathic nerve pain.
Mindbody Nerve Ischemia
Some patients diagnosed with pinched nerves are actually suffering from a far more logical and common type of symptomatic syndrome. Oxygen deprivation due to a psychosomatic back pain condition is the true cause of some of these misdiagnosed compressive neuropathy scenarios.
Oxygen deprivation has severe effects on ultra-sensitive nerve tissue and can affect them much in the same way as acute compression from a structural source. Ongoing chronic nerve pain and related symptoms make much more sense being caused by the variable process of ischemia, then from the static theory of anatomical compression. If you are suffering from chronic nerve related pain that has proven to be treatment resistant to a variety of therapies, consider the chance that your condition might actually be a case of misdiagnosed oxygen deprivation. Understand the pain in order to beat the pain.
Other cases of misdiagnosed compressive nerve conditions may have purely structural sources, as well. There are countless possible reasons for patients to experience neck or back pain and many patients have idiopathic suffering. To better your chances of avoiding misdiagnosis, always seek clinical correlation with a qualified spinal neurologist whenever the possibility of a pinched nerve is suggested as a potential cause of your symptoms.




