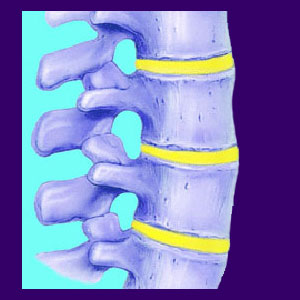
Facet joint arthrosis is another of the many terms used interchangeably to describe the diagnosis of facet syndrome. The arthritic processes affect the spinal facet joints, just like they affect virtually every other major joint in the body to some degree. It is normal to experience facet joint degeneration as we age, including the usual occurrence of structural changes which may be visible on spinal MRI studies. Being diagnosed with arthritic changes in the facet joints should be of no surprise to anyone of middle age or older. It is crucial to understand that arthritis in normal and expected in the various regions of the lumbar and cervical spine.
All these facts aside, facet deterioration is a commonly implicated cause of back pain, even when no evidence of pathology exists. This article explains why facet arthopathy is one of the most misunderstood of all dorsopathy villains.
What is Facet Joint Arthrosis?
Osteoarthritis is the underlying process which affects our joints as we get older. Arthritis is not inherently painful and is certainly not the usual source of severe or chronic symptoms in the facet joints. In some cases, arthritic change can create the ideal circumstances for pain to occur, but many cases of suspected facet joint syndrome are misdiagnosed.
Facet joint degeneration includes the breakdown of the protective measures in the joints themselves, including loss of synovial fluid and cartilage, as well as the possibility of problematic bone spur growth. Remember, in order for an osteophyte complex to create pain, it must be specifically located in an area which prevents normal joint function or impinges on a neurological structure. In many patients neither of these points are validly demonstrated.
Facet Joint Symptom Facts
Facet joint syndrome is almost always a mechanically-motivated back pain syndrome. This basically means that symptoms are brought on by specific movements and pain should not exist when the joint is not being aggravated. Chronic ever-present facet joint pain is almost always incorrectly diagnosed, as it generally goes against the principles which are capable of enacting pain in this location.
While almost all of us experience progressive deterioration of the actual facet joint structures, very few of us actually suffer any pain from these changes. This is one of the many reasons why facet joint syndrome is a terrific back pain scapegoat, since it is almost always present in patients 40+ (often much younger) and can be blamed for many different types of pain.
Facet Joint Arthrosis Considerations
Patients who have specific and logical symptomatic expressions supporting their facet syndrome diagnosis may have 2 options: They can wait for the arthritic osteophytes to possibly wear down using physical therapy and working through it (a speculative bet, at best), or possibly undergo surgical removal of the offending structures.
Of all the back surgery procedures, the ones used for facet arthritis are minimally invasive and typically successful for scenarios in which a bone spur is the definite cause of pain. Remember, this case profile is rare. The rest of you with chronic back pain blamed on facet joint degeneration may be wise to reconsider the validity of the theory, especially if the pain is not mechanically-motivated. This is particularly true if the symptoms affect a large area or move about due to position, activity or any other factor.
Our proprietary pain relief program has helped countless people recover from severe facet joint pain. The program is available to help you 24 hours a day, from anywhere in the world.



