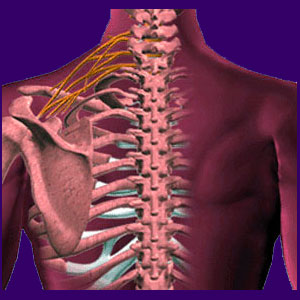
A herniated cervical disc can be a common result of a neck injury or a degenerative upper spinal process. Intervertebral discs break down, lose height and occasionally rupture as a normal part of their lifespan. Most herniations are due to normal deterioration of the intervertebral structures and should not cause any pain. This is clinical fact. However, it does not describe every possible disc pathology, since some can be mildly uncomfortable or even terribly excruciating for a time.
Sudden disc injuries can be acutely agonizing, although they are rarely to blame for ongoing chronic back pain conditions. In fact, research has shown that most symptomatic disc herniations will heal and stabilize on their own, without any medical treatment.
Research also shows that many disc protrusions are unfairly blamed for causing back and neck pain. Since intervertebral pathologies are the most common of all spinal irregularities, herniated discs are obviously the most common of all back pain scapegoat conditions. Remember this if you have been diagnosed with a minor to moderate disc issue. This knowledge may save you from years of unneeded treatment and possibly even unnecessary neck surgery.
This dialog delves into cervical intervertebral herniation and its possible consequences on the form and function of the neck.
What is a Herniated Cervical Disc?
The cervical spine is also called the neck region. It is responsible for supporting and facilitating movement for the head. The head is a heavy weight which can apply tremendous force on the cervical spinal structures in certain situations.
Whiplash is a perfect example of how the weight of the head, combined with sudden traumatic acceleration, can produce devastating anatomical effects in the neck.
Herniated discs in the neck occur when the outer wall of one or more of the cervical intervertebral discs is compromised. The outer wall helps to maintain disc shape and integrity. Once it is herniated or ruptured, the nucleus of the disc will bulge outward or even leak from the disc structure. This disc material is often blamed for causing pinched nerves, but that occurrence is actually quite rare.
Causes of a Herniated Disc in the C-Spine
Any traumatic injury to the neck region can cause significant disc damage. The vertebral structures in the neck are lighter and thinner than in the rest of the spine. It does not take tremendous force to inflict a nasty injury to the cervical region.
Herniated discs can also occur due to completely normal and virtually universal processes such as cervical degenerative disc disease. It is expected that discs will lose height and dry out as we age. Both of these processes can cause a weakening of the outer disc wall, possibly resulting in a herniation.
Degenerative disc herniations are not likely to be or become painful. Traumatic herniations may be symptomatic, but usually resolve in a short time expectancy. Only a small percentage of disc pathologies will enact lasting pain or neurological symptoms. However, when central spinal stenosis, neuroforaminal stenosis or chemical irritation does occur due to a particularly problematic disc concern, then symptoms may endure until resolved through proper diagnosis and effective treatment. In some of these cases, disc surgery may be truly needed to enable recovery.
Cervical Herniated Disc Guidance
The very diagnosis of a problem in one of the cervical discs is often enough to cause symptom escalation in many patients. We have all heard horror stories about disc pain and the devastating effects it has on the lives of hapless victims. Unfortunately, most people do not know the complete picture when it comes to herniated disc pain. Most disc herniations are completely asymptomatic and will not cause pain now or in the future.
A large percentage of the general population has herniated discs but does not even know it. The reason why so many apparent disc injuries have a bad reputation for becoming treatment resistant has little to do with the severity of the actual injury, but instead has far more to do with the common misdiagnosis of the actual reason for the pain.
If you have been diagnosed with a herniated cervical disc, learn the complete story of disc injuries yourself before agreeing to any ongoing or drastic back pain treatment modalities. Make sure to get several diagnostic opinions before pursuing any type of care at all, sine most herniated cervical discs are misdiagnosed as a actual origin of pain.




