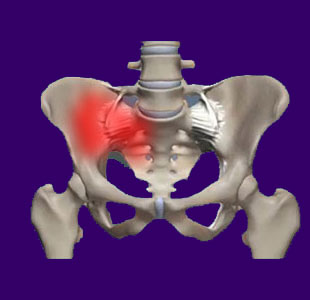
Sacroiliac joint injury can occur due to trauma, disease, surgery or even the effects of structural degeneration. Regardless of causation, injury to the SIJ can have horrific effects in terms of pain and functional disability, especially during weight-bearing and ambulation activities.
The sacroiliac joint is not immune to injury, just like every other anatomical location. They joint is very resilient however, and is not typically the site for traumatic damage compared to other local structures, such as the hip and lower lumbar spine. However, when injury does affect the sacroiliac joint, treatment can be difficult and is not always successful in the short-term.
This essay explores various types and circumstances of sacroiliac joint injury. We will explore the causes, symptoms and treatments for injury to the SIJ and help patients to make more informed healthcare choices.
Sacroiliac Joint Injury Causes
Injury is a general term for damage to the joint caused by known or unknown circumstances. This makes the definition far broader than simply direct trauma to the joint. In fact, direct trauma to the SIJ is one of the least common causes of injury, since the pelvis will typically shatter before the joint itself will be damaged. Remember that the sacroiliac is one of the strongest of all bodily joints. In cases of traumatic joint injury, the circumstances are usually extreme, such as significant falls from heights, car accidents, acts of violence and other catastrophic occurrences.
More common causes of sacroiliac injury include all of the following scenarios:
Structural degeneration might cause abnormal degrees of deterioration n and around the SIJ, consisting of osteoarthritic changes that can become painful in rare instances. While arthritis in the sacroiliac is normal to experience as we get older, symptomatic versions of OA are very rare.
Surgery on the sacroiliac joint, hip or lower back can all influence joint functionality directly or indirectly. Spinal fusion in the lumbar region is known for causing many sacroiliac joint problems within a few months to a few years postoperatively.
Disease can attack the sacroiliac joint and cause trauma. Autoimmune conditions tend to favor targeting the joint and might include such notable conditions as rheumatoid arthritis and ankylosing spondylitis.
Joint dysfunction results from soft tissue pathology affecting the ligaments which regulate joint movement. Hyperlaxity or excessive tension in the joint can both spell problems for affected patients, with pain and functional impairment being the most common consequences.
SIJ Injury Symptoms
Symptoms of sacroiliac joint injury will depend on the severity of damage and the type of causative condition present. We detail all the possible sacroiliac joint symptoms elsewhere on this website, but generally, the usual expressions will be similar regardless of cause:
Pain might be present in focal or general areas in and around the joint, including the lower back, hip, pelvis and upper leg. Some patients might also suffer tingling, weakness or numbness in the same areas. Symptoms will likely be worse with certain ranges of motion and during weight-bearing and ambulation. Rising from a seated position and sitting back down might be especially painful.
Patients will likely demonstrate pain during various diagnostic testing methods for SIJ dysfunction, including the Gaenslen Test, the iliac gapping test, the iliac compression test, the FABER or Patrick Test and the thigh thrust sacroiliac test.
Symptoms might be unilateral or bilateral, but experiencing SIJ issues on one sides does increase the likelihood of suffering bilateral symptoms eventually.
Sacroiliac Joint Injury Treatment
The best path towards successful treatment for SIJ injury depends on the causative condition responsible for the suffering. Each underlying origin of symptoms might have a very different preferred therapeutic course, so accurate diagnosis of this true cause is of paramount important to satisfying treatment.
Direct trauma to the joint might actually be the easiest to rectify and tends to heal the best given proper and timely care.
Soft tissue conditions causing sacroiliac joint dysfunction are largely unpredictable in how they will respond to treatment, especially since misdiagnosis of these issues is a common occurrence.
Disease processes causing SIJ symptomology should be managed by specialists in the underlying causative condition, often a rheumatologist in cases of autoimmune disease.
Structural degeneration is not a typical reason for symptomology, but in the rare cases where excessive deterioration of the joint is truly to blame, fusion surgery typically represents the best curative statistics, while conservative methods of care will not provide a cure but can help most patients to function better for extended timelines, allowing them to avoid surgery.




