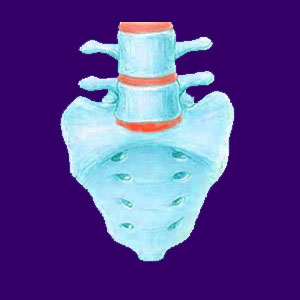
The sacrum is the region of the spinal column below the lumbar spine and above the coccyx. This spinal structure usually consists of 5 fused vertebrae acting as one solid piece of bone. These vertebrae do have individual names, S1 to S5, but sometimes the entire region is simply referred to as S1. This area is also called the sacral spine.
The sacral region is separated from the lumbar area by the lumbosacral disc, also named L5/S1. This disc is the #1 problem area for the majority of back pain sufferers. It has the distinction of being the most often degenerated and herniated intervertebral structure in the entire spine. This disc deterioration also facilitates an active arthritic response in most adults, with almost all mature people over age 40 demonstrating some degree of noticeable arthritic activity at and around the lumbosacral juncture. The actual sacral area itself is extremely strong and hard to fracture or injure, except in cases of extremely focused trauma.
This narrative explains the human sacral spine and the problematic conditions that affect it.
Anatomy of the Sacrum
The sacral spine is designed to bear weight, as well as join the spine to the pelvis. A normal sacrococcygeal spine is naturally designed to have a pronounced kyphotic curve.
The sacral spine is shaped noticeably different in men and women. In women, the structure is usually wider and shorter to facilitate childbirth. These anatomical differences can help in the gender identification of bodies from skeletal remains.
The sacral spine is located between 2 problematic regions, including the lumbar spine and the coccyx. However, the sacral region itself is rarely the source of pain, since it is super strong and not separated internally by intervertebral spacers which are noted as being one of the main pathological components featured in every other spinal area.
Sacral Lower Back Pain
Many of the nerves in the sacral spine are implicated in causing low back pain and sciatica. Being that the foraminal openings are virtually always patent in the sacral structure itself, this means that most cases of compressive neuropathy occur higher in the lumbar spine when these nerves exist freely as part of the cauda equina. In many instances, a central spinal stenosis process can affect the viability of these nerves in the lower lumbar spine or at the lumbosacral juncture.
The sacral spine is rarely directly implicated in causing low back discomfort. The exception to this rule is when the area is theorized to be tilted out of alignment, which is most commonly a diagnostic theory embraced by chiropractors exclusively.
The other major cause of possible sacral pain is direct traumatic injury, which can even fracture the sacral structure in the worst circumstances.



