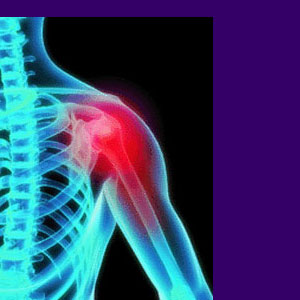
Shoulder bursitis is one of the most prevalent forms of diagnosed bursa-related pain. In the shoulder joint, there are four tendons which make up the rotator cuff. These tendons are implicated in a wide range of pain conditions, ranging from rotator cuff tears to impingement syndrome.
In the case of bursitis of the shoulder, almost any of these tendons may be affected by inflammation, although the most common one linked to most painful complaints is the supraspinatus tendon, which is located at the top of the shoulder joint.
It is crucial to understand that bursa degeneration is normal throughout the body and most patients will never experience pain from this process. Research shows that shoulder pain is often idiopathic and cannot be traced to a definitive source condition. Meanwhile, many patients with truly advanced degeneration in the shoulder joint have no pain whatsoever.
Let’s investigate why shoulder bursitis is just one of many regional pain syndromes that is often mistakenly diagnosed as the true origin of pain.
What is Shoulder Bursitis?
Just like all forms of bursitis, inflammation of the bursa in the shoulder can cause pain due to friction inside the moving parts of the joint. There is no doubt that people with advanced osteoarthritic changes in the shoulder may experience some amount of pain, especially during certain specific movements. This is due to the wearing away of the normal protective mechanisms in the shoulder joint itself and the loss of synovial fluid from the bursa sac.
Of course, just like other forms of bursitis, the condition exists in almost all of us, as we age, yet is only painful in some. Misdiagnosis of supraspinatus bursitis is rampant, with many patients suffering from completely different causes for their pain.
Causes of Bursitis in the Shoulder
Like all other types of bursa change, painful bursitis can occur from extreme joint degeneration and be based completely on structural anatomical issues. However, many people demonstrate the exact same level of deterioration in the joint, yet have no pain.
Many patients who are diagnosed with bursitis, torn rotator cuffs and impingement syndrome are actually suffering from regional ischemia of the soft tissues in the shoulder joint, including the tendons and muscles. This is very common, but seldom correctly identified as the actual source of pain, leading to failed treatments and unsuccessful surgeries in many cases.
Rheumatoid arthritis and other autoimmune disorders can also play a role in shoulder bursa issues, further linking the condition to the mindbody process in many patients.
Shoulder Bursitis Factsheet
Be very careful about undergoing drastic or invasive treatments for shoulder issues without careful consideration. Many doctors recommend surgery, which is sometimes inappropriate and ineffective. Many patients see no relief from these procedures, while some see partial relief or full temporary relief.
Other patients enjoy resolution of their pain in the shoulder, only to have it come back in a nearby location, such as the bicep or forearm. This is a usual sign of psychosomatic causation, when the anatomical changes act as mere scapegoats for the pain.
The point is simple: Rotator cuff tears, bursitis and osteoarthritis are common in the shoulder and only cause severe and lasting pain is rare instances. Be wary of symptoms which seem too significant to be explained from mild or even moderate degenerative changes. Never rush into treatment without research and always exhaust all conservative measures before even thinking about surgical interventions.
Our proven pain relief program is particularly effective for resolving shoulder pain and has saved countless people from undergoing unnecessary shoulder surgery.
Back Pain > Psychologically Induced Pain Syndromes > Shoulder Bursitis



