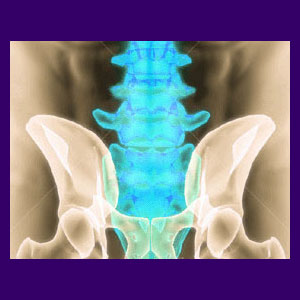
Spina bifida occulta is a developmental spinal abnormality which involves one or more vertebrae featuring abnormal holes in the rear surface of the bone. Occulta is sometimes blamed for sourcing a host of back pain conditions, mostly illogically and unfairly. Statistics clearly show that most cases of occulta are not symptomatic and will not cause any problematic concerns for affected individuals.
Occulta is a very common birth defect and often exists in the spine without the person even knowing of the condition. So many patients find out they have had occulta their whole lives when it is discovered during coincidental and unrelated spinal imaging later in life.
This essay focuses on providing an objective view of bifida occulta to help diagnosed individuals better understand their conditions.
What is Spina Bifida Occulta?
Occulta is typically the mildest form of spina bifida. The condition is characterized by one or more vertebrae which have not formed correctly. The typical profile demonstrates small openings in the outer surface of one or more of these spinal bones. These openings vary in size, but are not large enough to allow the spinal cord to protrude through the protective barrier provided by the spine.
Occulta has not been proven to contribute to any form of back pain, but is typically implicated as a scapegoat when symptoms exist coincidentally with the condition.
It is no surprise that given the nocebo effect of being diagnosed with holes in vertebral bones, many patients suffer an escalation of symptoms immediately afterwards, especially when the doctor does not tell them of the mostly innocent nature of the occulta condition.
What Causes Spina Bifida Occulta?
This developmental vertebral column abnormality occurs during the very first month of fetal growth. The condition is mostly idiopathic in nature, but certain contributing factors have been positively identified. Some of the more common causative factors include:
Occulta is more likely in female children than male.
Genetic contributing factors can contribute to any form of bifida.
Poor health during pregnancy can increase the risk of spinal bifida.
Having an obese or diabetic mother increases bifida likelihood.
Increased risk if mother demonstrates lack of folic acid in diet.
Pharmaceutical use during pregnancy, especially some anti-seizure drugs, ups the risk of developing vertebral holes.
Although these circumstances can increase the chance of spinal bifida in a fetus, most cases are caused by unknown factors.
Bifida Occulta Prevention and Treatment
Occulta is virtually never symptomatic and should not require any special back pain treatment. Serious versions of the condition should be monitored by a qualified physician, although actual intervention is rarely necessary.
Preventing the condition is usually quite effective and consists mostly of eliminating risky pharmaceutical products and increasing folic acid intake. Folic acid is found naturally in whole grains, beans, leafy vegetables and fruits. It can also be consumed as a nutritional supplement. The condition can be discovered very early in fetal development through blood tests and high resolution ultrasound testing.
In rare cases, some women have chosen to terminate pregnancies of fetuses found to have bifida. This is especially true for cases of bifida cystica, also known as myelomeningocele, which is a far more severe condition than occulta.
Spina Bifida Occulta Factsheet
Although most cases of occulta are completely harmless, there are some which might be problematic. The higher the level of affected vertebrae and the larger the opening in the outer surface of the spinal bones, the greater the chance of experiencing a symptomatic condition.
Tethered spinal cord syndrome is sometimes experienced by some patients in addition to occulta and might be to blame for neurological impairment. This additional condition may or may not be related to the occulta deformity.
The vast majority of patients with occulta should not expect any symptoms from this mostly benign spinal irregularity. Unless you are in the small percentage of symptomatic patients, do not allow any doctor to frighten you with a diagnosis of occulta.
The nocebo effect of poor bedside manner will certainly create symptoms in some patients. In these cases, the pain is obviously psychogenic and should be treated with a combination of education and knowledge therapy.




