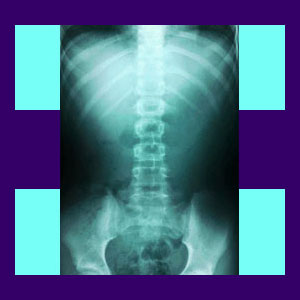
Spinal x-ray is one of the main diagnostic tools used throughout the medical professions to ascertain the potential causes of a back pain complaint. X-rays can be very helpful for diagnosing some skeletal conditions, but are completely ineffective at determining the definitive cause of most back ache syndromes.
X-rays are limited in the types of tissues they can accurately image. Furthermore, doctors can use x-rays to implicate spinal scapegoat conditions which may be atypical, but are rarely problematic or painful.
Recent revisions to diagnostic policy instituted by many major medical associations have advised doctors to stop relying exclusively on x-ray or MRI to diagnose back pain directly, since most structural irregularities demonstrate no link to the existence of back ache and must always be studied to be sure conclusive proof of a pathological process exists.
Spine X-Ray Facts
X-rays will clearly visualize the vertebral bones in the spine. This is helpful to determine if there are any fractures or large build ups of osteophyte material around the vertebral bones.
X-rays are very useful for diagnosing scoliosis and other forms of spinal curvature, such as lordosis and kyphosis.
Side view x-rays will generally show noticeable levels of spondylolisthesis.
X-rays will also show the signs of degenerative disc disease, since the vertebral bones will be closer together at affected levels. However, x-rays will not reveal the extent of disc degeneration or herniated discs, nor will they show any potential neurological effects on the patient.
X-rays will not visualize any soft tissue condition, such as back muscle pain, piriformis syndrome or fibromyalgia.
Spinal X-Ray Concerns
When used appropriately, x-rays are a great tool in a doctor’s arsenal. However, many times, they are used to make a diagnosis which can not be accurately confirmed without the use of a more advanced imaging study, such as an MRI. This is most commonly seen in the diagnosis of herniated discs, since the patient will have pain and also demonstrate a clear thinning of disc height in the affected region.
X-rays alone should never be used to paint a clinical picture of any soft tissue pathology, including any intervertebral disc issue. Doing so will only increase the already high percentage of patients whose pain is obviously misdiagnosed.
Spinal X-Ray Conclusions
My first chiropractor took x-rays and used them to reinforce the significant nocebo effect he imparted upon me due to his poor bedside manner when presenting the diagnosis. He used many frightening words such as “degenerated”, “bent spine” and “chronic pain” to set the stage for what would become 18 long years of suffering. I can remember that my x-rays did not seem to look that bad to me, but certainly made a big impression on this chiropractor. Looking back, he saw me as a cash cow and milked the opportunity for all it was worth.
If you have x-rays, that is great. If you have been diagnosed with a bone condition from your x-rays, then they have proven themselves to be very valuable indeed. However, if you do not have a diagnosis, or worse yet, have a soft tissue diagnosis as a result of an x-ray, make sure to insist on an MRI, if at all possible. This imaging study will better detail the affected area of your spine and give both you and your doctor a better view of what is truly going on in your back.
It is crucial to remember that even MRI can only provide detailed pictures, never a diagnosis. All diagnostic films are subject to interpretation, which explains why so many patients never achieve an accurate verdict as to what is truly causing their pain.
Subjectivity of evidence is a huge problem in the back pain treatment sector and what one doctor sees as completely normal and innocent may be another doctor’s excuse to place a patient into immediate surgery. Never forget that medicine is often a science of opinion… not always objective fact.



