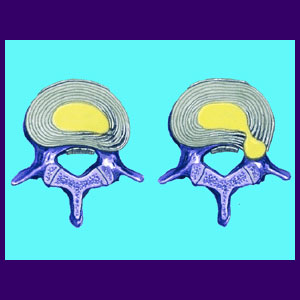
An annular tear describes a hole in the outer intervertebral tissue wall, possibly facilitating the expulsion of nucleus pulposus material from the disc into the greater surrounding spinal anatomy. Annular tears are relatively common in the intervertebral discs and are not inherently painful or pathological in any way. Annular fissures can create pain and neurological effects in some patients through various mechanisms, but these cases are not commonly seen.
This treatise explains holes in the annulus fibrosus that compromise the structural integrity of intervertebral discs. We will detail what causes these holes to occur, as well as the consequences of suffering an annular fissure in one or more spinal disc tissues.
Traumatic Causes of Annular Tear
Annular fissures can occur for several known reasons, but most are considered idiopathic occurrences. Unless before-and-after imaging is available for comparative analysis, it is virtually impossible to determine if a particular event directly caused an annular injury or not.
Trauma is the most logical causation of known annulus fibrosus injury. Damage can occur from any sudden and significant disc injury, such as car accidents, falls, sporting traumas or acts of violence. If tremendous stress is placed upon the annulus fibrosus, it is certainly possible to buckle under the pressure and suffer any degree of hole formation ranging from a tiny crevice to a complete open rupture, extrusion and sequestration of the entire nucleus pulposus.
Spinal surgery is another common cause of annular injury, with many procedures being implicated in creating holes in the spinal discs. Discectomy techniques are the most prevalent culprits, but even practices that do not specifically target the intervertebral tissues, such as laminectomy, can be causative. Minimally invasive practices, such as nucleoplasty and IDET are equally guilty of potentially creating holes in the annulus that do not heal. Finally, certain types of injection therapies might also provide the catalyst for an annular fissure to take place.
Degenerative Causes of Disc Wall Tear
Most annular fissures develop for idiopathic reasons that are typically related to the usual degenerative aging processes. The normal life timeline for spinal discs involves desiccation and subsequent breakdown of the disc, including reduction in the mass of the nucleus and decreased hydration of both the nucleus and the annulus.
A degenerated annulus fibrosus is more likely to crack, especially when placed under the type of stress that is inherently borne by the spinal structures. No anatomical structure is immune for the ravages of age and activity and the annulus fibrosus is certainly no exception to this rule. Just like anywhere else in the anatomy, as we get older, the annulus has a greater chance of failing to contain the nucleus, maintaining perfect and youthful spinal disc stability.
This aging process has been ridiculously named degenerative disc disease by some physicians, but this is a terrible misnomer. Disc degeneration is not a disease and is a completely universal finding in adult spines. This is why we prefer to use the objective and factual descriptive term intervertebral desiccation, as this nomenclature does not impart the same diagnostic nocebo effect on patients that can create, escalate or perpetuate pain.
Annular Tear Consequences
Most annular fissures will not significantly reduce the functionality of the disc, as they are small and might not go through every layer of annulus tissue. For fully-formed holes, some amount of nucleus material might be able to leak out of the disc. This nucleus tissue is what is thought to cause trouble in most cases of painful annular rupture.
In some instances, large amounts of nucleus tissue might be ejected, possibly under pressure, against the surrounding neurological tissue, including the spinal cord and/or nerve roots. This leaked tissue might cause or contribute to central spinal stenosis or neuroforaminal stenosis in some patients, possibly eliciting symptoms.
In more cases, leaking nucleus tissue is thought to create symptomatic expressions through a process known as chemical nerve irritation, also known as chemical radiculitis. This is a highly debated diagnosis, since only some people seem to demonstrate a painful sensitivity to a substance found in the nucleus proteins, called tumor necrosis factor alpha.
In most instances, an annular fissure will not create pain, nor even be known to the affected person unless it is discovered inadvertently when performing incidental diagnostic imaging for some other health issue.
Spinal Disc Tear Treatment Options
Most annular holes will not be treated logically, even if they are suspected of causing pain. Diagnosed patients are often instructed to undergo a variety of conservative methods of care which are certainly profitable, but quite pointless from a scientific point of view.
Remember, an annular tear is a hole in the spinal disc wall deep inside the body. No conservative therapy will fill this hole, nor cure the pain that is theorized to be coming from this source. Physical therapy, chiropractic, drug therapies and a host of complementary practices all seem useless in treated annulus fibrosus tears, yet all of these treatments are commonly utilized for this very purpose.
Epidural flushing injections are logical as a treatment for chemical radiculitis and often are quite effective in relieving verified neurological symptoms linked to tumor necrosis factor alpha exposure.
There are also several existing surgical techniques, such as IDET and nucleoplasty, that have been specially modified to seal annular cracks and tears. These procedures are typically performed by a select number of specialists in large medical markets in the most developed regions for healthcare infrastructure. Finally, some fully invasive techniques, such as discectomy, disc replacement surgery and spinal fusion might be utilized to surgically treat discs that might have caused chronic pain problems that have not responded to more conservative and moderate therapy approaches.




