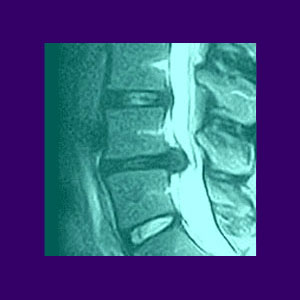
A back pain MRI is the most useful of all diagnostic testing procedures used to ascertain possible structural causes for a chronic dorsopathy complaint. However, not all is positive when it comes to magnetic resonance testing. This is because although the test itself is virtually risk-free and incredibly precise, the results must be subjectively interpreted by a radiologist. This can lead to some serious problems when it comes to achieving a true and correct diagnosis of the actual source of pain, versus simply recognizing the structures which might be deemed atypical.
Magnetic resonance imaging provides ultra clear and detailed pictures of the spinal structures from various angles, allowing doctors an unprecedented look inside the body to observe the spinal column from every possible vantage point. In fact, when pieced together, the various images of an MRI can create a virtual three dimensional model of the spine.
Back Pain MRI Benefits
MRI is a fantastic technology which will detail all the spinal structures, including bones, discs, and some neurological tissues. MRI is far more advantageous to both doctors and patients alike, when compared to more common back pain x-ray films, which show little detail, except bone.
MRI will provide some insight as to the possible source of symptoms in the spinal column and may help to rule out possible causations, as well as narrow the field of suspected culprits. When it comes to confirming or excluding structural issues which may or may not be responsible for enacting pain, there is no beating MRI technology. No other test can produce such accurate and detailed images, helping patients to better understand exactly what is occurring inside their vertebral columns.
Back Pain MRI Problems
Although the MRI will detail the spine and show any irregularities which exist, there is no way to determine if these spinal abnormalities are indeed responsible for enacting pain from the test itself. In fact, statistics show little, if any, correlation between most spinal structural irregularities and the incidence of back or neck pain.
Although most of the common abnormalities, such as spinal arthritis and herniated discs, are often blamed for creating pain, there are many people with identical structural issues who endure no pain whatsoever. Meanwhile some people have dire and chronic pain, yet do not present any unusual MRI findings in their spines. It is no wonder that many medical organizations have now warned member physicians never to utilize MRI results as an exclusive diagnostic tool without performing all the other intrinsic steps, such as clinical symptomatic correlation and neurological testing.
Back Pain Magnetic Resonance Imaging
Remember that some, if not all, of the structural issues detailed on an MRI report will be coincidental to the pain and not the direct source of it. These are called back pain scapegoats and are the primary reason for the epidemic misdiagnosis of dorsalgia symptoms in the healthcare system. Sure, the irregularities are there, but they do not cause any pain in most instances.
Remember also that many spinal abnormalities are discovered via imaging after a traumatic accident. There is pain from the trauma and many times, a herniated disc, or other irregularity, will be noted on the film and blamed on the recent injury. However, these abnormalities often existed there long before the accident and were not caused by the event. The condition never caused pain before and does not cause pain now. This is why it is crucial to go to a spinal expert who can decipher old abnormalities from new fresh occurrences. Degenerative changes in the spine will make these distinctions obvious to those who know what to look for.
It is vital to know that MRI never diagnoses anything. Instead, the images must be read by a doctor in order to produce a diagnostic verdict. Being that this is an incredibly subjective process, it is no wonder that patients may never really know the validity of any proposed theory of pain. It is very common for patients to take the same films to several doctors and get very different diagnostic pronouncements from each. This mirrors my own experience in the back pain treatment sector. Even now, with a total of 12 herniated discs in my spine, I still do not have a verified diagnosis which explains my past symptoms…



