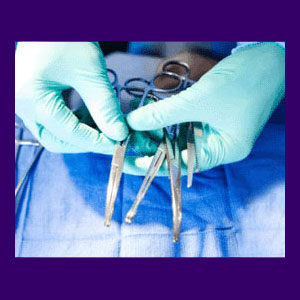
Back pain caused by surgery is a common consequence of invasive dorsalgia care and can even occur from many unrelated surgeries that do not involve the spine. We have been writing for more than 15 years about how so many spinal surgeries might seek to heal and provide relief in theory, but fail to do so on a practical level. However, we rarely talk about how many general surgeries are also responsible for causing back pain, even when none was present prior to the operation.
Surgery is a barbaric practice wherein patients are literally cut open and dissected. Sometimes, plastic or metal components are placed into the body, while other times, organic body parts are removed and discarded. There is no doubt that surgery has its applications in any modern medical system, but few would argue that surgical interventions are horribly overused, often inappropriately used, and are often unsuccessful for various reasons. Regardless of their overall safety or indication, surgery can create back pain, or worsen existing back pain, even when everything works perfectly and the operation is deemed to be a stunning success.
This discussion explores exactly how surgery can cause chronic pain conditions in the back or neck. We will focus on both the anatomical causes of this pain and provide answers on how it can be prevented. This essay serves as an addendum to our previous coverage on the subject of back surgery pain.
Back Pain Caused by Surgery of the Spine
Spinal surgery is certainly the most common direct medical cause (iatrogenic cause) of dorsalgia. The vast majority of spinal operations are performed in an effort to reduce or eliminate back pain or neck pain symptoms that currently exist or to resolve various symptomatic effects (tingling, numbness, weakness, dysfunction) caused by neurological compression. Some procedures are used for other purposes, such as correcting non-painful structural issues that threaten physical functionality or the internal organs, like severe kyphosis, lordosis or scoliosis. Meanwhile, other procedures are geared towards treating disease that might not create any back pain, such as cancer, or non-pathological but unaesthetic issues, such as large cysts. There are many possible indications for spinal surgery to be undertaken.
Regardless of the indication for spinal surgery, the techniques involved are always very risky and have the potential to cause extreme problems for the patient, even when the primary surgical goal is successfully enacted. Some of the major collateral consequences of spinal surgery that can directly create or contribute to back pain include all of the following factors:
Nerve damage is very common and can occur to the spinal cord, spinal nerve roots or any of the peripheral nerves that grow from the neural roots. Nerve damage can cause pain, although chronic pain is not common. Instead, injury to nerves usually results in the diminished ability to signal correctly, often creating areas of numbness and weakness in the anatomy that might be transient or permanent.
Soft tissue damage can occur to the back muscles, ligaments, tendons or cartilage. Sometimes, it is unavoidable to damage these tissues during operations, due to dissection that must be utilized, while other times, damage is not inherent and is considered negligent. Soft tissue damage can manifest as pain or functional problems and might last long-term or forever.
Scar tissue can form on any of the tissues that are exposed to trauma during the procedure. Scar tissue has certainly become a great scapegoat in the arena of medical explanations for pain, but is very real and can create symptoms when it affects tissues involved in motion or nerve signaling.
The inherent nature of some spinal surgeries makes them prone to be pain producers. This is especially true of operations that seek to change the way the spine works or is formed, such as spondylodesis, implant placement techniques or corpectomy.
These are just some of the many structural reasons why surgery might produce chronic suffering even after healing is complete.
Back Pain Caused by Nonspinal Surgery
Similar to spinal surgery, other types of operations can also create back or neck pain that might endure chronically. This is true even if the procedure does not influence the immediate anatomy surrounding the spine. We can still cite many examples of scar tissue, nerve damage and soft tissue damage that might directly affect tissues in the dorsal anatomy as potential causes. However, there are also other symptomatic source possibilities that might not be considered by many patients or their care providers:
Organ damage is often felt in the rear of the body and might be mistaken for back pain. This is commonly seen in kidney procedures, lung procedures, heart procedures, pancreas procedures and stomach procedures. It is less often seen, but still possible from other surgeries, including those of the liver and gall bladder. Many of these organ-related pain syndromes will eventually resolve or drastically improve, but some will become chronically symptomatic.
Muscles work in sets throughout the body and even when damage is done to a muscular tissue on the anterior face of the anatomy, it can affect the way muscles on the dorsal face work through various interactions and compensations. The results of muscular damage might include imbalances that create overly strong and overly weak matched pairs. This can be a cause of long-term back or neck pain and is rarely correctly linked to the source procedure.
Ischemia can result when circulatory vessels are purposefully or accidentally treated during any type of operation. Circulatory patterns can be wide ranging and might affect the blood supply to tissues in the dorsal anatomy, including the spine, muscles or superficial tissues.
Prevention and Treatment of Back Pain Caused by Surgery
The easiest way to prevent back or neck pain from an operation is simply not undergoing the surgery. While this seems like obvious advice, it is amazing how often it is not heeded, despite there being no medical indication for the surgery to begin with. The vast majority of spinal operations are not necessary, nor are they even rated as being effective for the conditions targeted. This includes spinal fusions, discectomies, laminectomies and the wide range of minimally invasive practices like IDET and nucleoplasty. Very few patients actually must undergo any type of spinal surgery and only a minority of patients enjoy lasting relief from whatever pain they currently have after spinal surgery. However, a fair percentage of patients have new pains brought on by the surgery, while an even larger number cite symptomatic escalation of their old complaints postoperatively.
Surgeries outside the spinal anatomy are often elective, as well, or performed prematurely for conditions that do not objectively require invasive care. Barring life-saving techniques, many internal operations on the torso are deemed truly unnecessary by objective medical observers.
Therefore, the easiest way to prevent pain from occurring after an operation is to avoid the procedure altogether. If this is an option, then consider it carefully before going under the cruel surgical knife. If not, then you might have to take your chances and try the following preventative strategies to minimize your risks:
Choose the least invasive surgical approach that will still satisfy the objective of the procedure. Less anatomical damage is always better, will heal faster and will pose less risk for immediate and eventual complications.
Choose the very best doctor who is available to you. Never simply meet with a surgeon and allow them to operate on you without a thorough investigation of their credentials, surgical record, history of litigation, complaints and professional disciplinary actions. Try to speak to former patients who already had your chosen operation for references.
Be sure to question the doctor about the surgical plan and try to limit their ability to suddenly decide on elective aspects of an operation to make things easier or faster for them. For example, many spinal operations provide a clause that the patient must sign, stating that the surgeon can elect to incorporate spinal fusion into virtually any procedure if and when they feel it is necessary. Now on the rare occasion when fusion is truly needed to save life or preserve spinal stability, this is warranted. However, this clause is routinely exploited by surgeons who simply want to have an easier time during the procedure or just want to make more money. It sounds unconscionable, but we have found it to be the truth in virtually every case where a patient undergoes a discectomy or similar technique and awakes with a fused spine and all the potential problems that accompany it.




