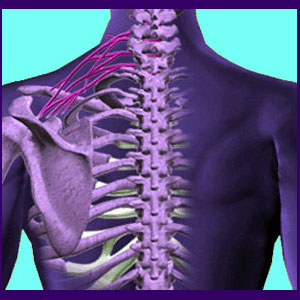
The brachial plexus is the network of neurological tissue which is composed of nerve roots originating from the C5, C6, C7, C8 and T1 vertebral levels. This region also contains some major vascular tissues which provide circulation to large anatomical targets. This is the group of nerve tissue which is often implicated as being compressed by the muscles of the upper back and shoulder, causing the condition known as thoracic outlet syndrome. There are neurological and vascular versions of thoracic outlet, each enacting frightening and potentially serious symptomatic expressions.
The scope of this article will detail the anatomical configuration of this upper body nerve center, as well as the occurrence of brachial plexus pain syndromes.
Brachial Nerve Plexus Definition
The BP is responsible for providing nerve energy to large areas of the upper body, including parts of the neck, head, shoulders, torso, arms and hands. There are also major circulatory structures in the region in the form of the subclavian artery and subclavian vein. Sometimes, these blood vessels are also implicated in arterial or venous thoracic outlet syndrome pain conditions.
Compression, oxygen deprivation or damage to the highly sensitive BP tissues will affect the upper body and especially the functionality of the arms and hands. Typical symptoms of trauma to any or all of the BP nerve structures include upper back pain, neck pain, tingling, numbness and weakness in affected areas of the upper torso or upper extremities.
If the vascular tissues are targeted, then the symptoms of ischemia will be apparent, including changes in the skin and possible systemic effects.
Brachial Plexus Information
A pinched nerve in the BP is a very common diagnosis. Although this scenario is possible and is more likely when obvious trauma is involved, many suspected instances of neurological thoracic outlet syndrome are very often misdiagnosed.
Be especially careful of chronic upper back pain or chronic neck pain which does not respond well to appropriate treatment options. This type of unresolved back pain often denotes a misdiagnosed symptomatic condition.
Regional ischemia of the BP area can produce alarmingly similar results to severe trauma and might exist for idiopathic reasons or due to the trigger effect from an accident or perceived back injury. For these cases, diagnosis can be difficult, since oxygen deprivation can occur here from true muscular compression of the subclavian structures by the scalene muscles, but may also be enacted by a completely distinct mindbody process.
Structural compression scenarios of either nerve or circulatory tissue must be treated medically. However, mindbody regional oxygen deprivation might respond better to a psychoemotional approach, such as that offered by knowledge therapy.



