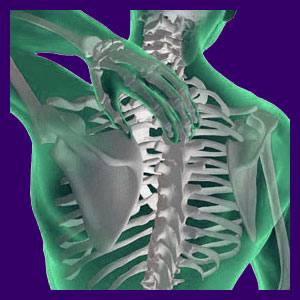
Thoracic outlet syndrome describes a condition of nerve or vascular tissue compression in the upper back and lower neck region. Although not linked to a spinal causation, the symptoms of the diagnosis can be almost virtually identical to any other type of compressive neuropathy which occurs inside the spinal canal.
TOS, as it is commonly called, is basically much like an upper back version of piriformis syndrome, in which a muscular structure is theorized to place considerable pressure on a major neurological center. In some cases, this compression can target an artery or vein instead of a nerve and may have similar or different symptomatic expressions.
Thoracic outlet syndrome is a diagnosis on the rise throughout the back pain industry. This condition is a controversial diagnosis, since it usually deals with nerve compression enacted by a muscular, rather than spinal source, and therefore it may not be possible to confirm via diagnostic imaging. Chronic pinched nerves are rarely caused by a structural non-spinal abnormality, as indicated in the TOS diagnosis, so patients are advised to be vigilant for signs of a misdiagnosed back pain syndrome.
This resource section examines the growing trend towards the diagnosis of thoracic outlet as an explanation for dorsal symptomology.
What is Thoracic Outlet Syndrome?
TOS is most commonly blamed on impingement of the various neurological structures which comprise the brachial plexus. The brachial plexus is a network of nerve tissue stemming from the spinal nerve roots at C5 through T1, which provides motor and sensory messages to and from parts of the neck, shoulders and upper back regions. This most often diagnosed form of the pain syndrome is called neurogenic TOS.
Less commonly, vascular tissue is implicated in the compression process, typically the subclavian artery or subclavian vein. This far less common cause of symptoms is referred to as arterial or venous TOS.
Occasionally, some patients might be diagnosed with both the neurogenic and arterial/venous forms at the same time.
Thoracic Outlet Topics
Thoracic outlet is a mysterious diagnosis for many patients. The following reports help patients to better realize the implications of TOS, before seeking treatment.
Thoracic outlet diagnosis is rarely made early on in the treatment process. Instead, most patients are labeled with other diagnoses first and eventually get a revised verdict of TOS once many therapies have failed to bring about relief.
Thoracic outlet treatment is mostly a conservative course of action for patients, but in drastic cases, thoracic outlet surgery may be employed to correct particular issues in the brachial plexus.
Brachial plexus pain and thoracic outlet pain are interchangeable names for the terrible discomfort associated with TOS conditions.
Pain between the shoulders is just one of the many possible symptoms of TOS.
Thoracic Outlet Syndrome Symptoms
Symptoms of TOS vary from patient to patient and from causation to causation. Typically, there is pain, stiffness and loss of mobility, functionality and range of motion in the neck, shoulder and upper back. There might be pain in parts of the upper chest or underarm region. Patients might also experience radiating neurological symptoms in the neck, shoulder, arms and hands, such as tingling, weakness and numbness. Arterial or venous forms of the condition might demonstrate a weak pulse in the affected arm and wrist.
Certain activities or postures typically worsen or relieve symptoms, although in many cases, this can merely be a conditioned response. TOS is more prevalent in woman than in men and is particularly common in athletes, office workers, people with bad posture and workers with repetitive motion jobs.
Read more about thoracic outlet symptoms.
Thoracic Outlet Syndrome Causes
Thoracic outlet syndrome can result from a back injury, such as sports trauma or a car accident. TOS can also come about gradually or spontaneously, even though no trauma has been endured. These idiopathic forms of TOS are even more likely to be misdiagnosed and sometimes even turn out to be regional ischemia syndromes caused by a psychoemotional process.
Abnormalities with the scalene muscles have been linked to thoracic outlet development, but this is no surprise, since medical science always looks to a structural source for all physical pain, even when the anatomical condition might be purely coincidental and innocent of symptomatic expression. Hypertrophy, overuse or injury to the scalene muscles does seem to have some bearing as to who might develop TOS, but is not a factor in all patients.
Read more about the causes of thoracic outlet.
Thoracic Outlet Syndrome Help
Thoracic outlet certainly exists, mostly due to obvious trauma. Even minor muscular injuries near the brachial plexus can cause TOS symptoms, although most of these issues should resolve in a few days to a few weeks. Long-term structurally induced TOS is rare and generally might indicate a possible mistaken diagnostic theory.
Tension myositis syndrome in the upper back and lower neck is generally diagnosed as TOS much of the time. Obviously, this leads to the treatment resistant pain which plagues the medical community, as patients continue to suffer despite a battery of seemingly appropriate, but unsuccessful treatment options.
Physical therapy and chiropractic are the most common conservative treatment options. Injection therapy is common as a next line of defense, along with the ever present pain management drugs which rule the back pain therapy industry. Surgery is sometimes used in extreme or chronic cases, but should be avoided unless there is no other option and the diagnosis is confirmed with 100% certainty.
As with many soft tissue pathologies which are almost impossible to prove and even harder to disprove, this TOS condition is extremely popular with care providers who are looking for reasons to keep their patients in ongoing, money-making treatment. Complete resolution of the condition is possible when the muscle is indeed the source, but being that many patients show chronic and ongoing pain syndromes in the brachial plexus, the most logical thought is that the causative process is not compressive, but ischemic in nature. Therefore, the usual therapy options utilized for care are not focused on the actual underlying source and do not work. Keep this in mind if your doctor claims TOS, but is unsuccessful in curing you.
Our proven Cure Back Pain Forever Program is perfectly suited for addressing thoracic outlet syndrome symptoms. If you need help right now, you will find all the program components online for immediate relief.




