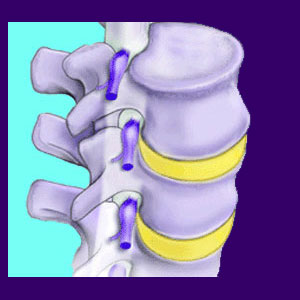
Degenerative joint disease is a spinal arthritis condition that is a normal part of the aging process. It is virtually universal and is not an inherently symptomatic condition. However, there are physical, circumstantial and genetic factors that increase the chance of a patient developing painful DJD. It must be noted that this condition, despite its fearsome name, is not a disease at all. Instead, it is a completely normal, expected and universal aspect of aging found in the lumbar, cervical and sometimes even thoracic regions of virtually every adult on this planet. Calling osteoarthritis a disease is like calling aging a disease… It is imply illogical and baseless.
This essay explores the origins of spinal joint degeneration and lists the most common contributing factors to serious cases of joint deterioration.
Degenerative Joint Disease Factors
The following are all factors which contribute to degenerative joint disease in the spine or cause it directly. As previously mentioned, simply being an aging human being will result in arthritis to some degree. There is just no way around this fact. However, the severity of arthritic change and possible subsequent symptoms vary greatly from patient to patient. Here are some factors to consider:
Aging and normal spinal degeneration are the primary causes of DJD. The condition usually affects people over 45 years of age, but can certainly be present much earlier in life, particularly in areas of the body which have been overused or abused. Arthritis can often be found in teenage gymnasts and competitive athletes in their twenties.
Women have a greater risk of developing DJD than men. The reason for this is idiopathic, but may be related to a less dense bone structure.
Genetics can influence the development of DJD. The genetic trait is commonly inherited, especially on the mother’s side.
Obesity can increase the chance for symptomatic DJD by up to 400%. Extra weight on the spine and joints will obviously be more stressful.
Repetitive strain can influence painful DJD development. This is especially true for heavy and difficult work. People who are involved in manual labor jobs will demonstrate arthritis earlier than sedentary people in most instances.
Back injuries can be starting points for symptomatic DJD to develop. Repetitive injuries to the same location are especially high risk for creating painful symptoms.
Degenerative Joint Disease Explained
DJD is caused by the erosion of cartilage around the spinal joints. A normal, healthy joint is surrounded by cartilage and is well lubricated by synovial fluid. Spinal facet joints degenerate due to normal wear and tear from a lifetime of use. When this degeneration occurs, the cartilage is damaged and the lubricating fluid in the joint becomes less effective. This causes increased vertebral surface contact.
Vertebral rubbing causes spurs, or osteophytes, to form around the spinal joints. These bone spurs can be painful, but are usually asymptomatic. Bone spurs are the second most commonly blamed source of foraminal stenosis in the spine, but are rarely the actual cause of pinched nerve conditions.
These same processes can occur in all the vertebral joints, as well as on the vertebral bodies themselves. In fact, the universality of disc desiccation will bring vertebral bodies closer together with age and activity, causing increased interaction between individual vertebral bones. This results in the same evidence of degenerative joint disease which is noted above, as well as the possibility for debris entering the central canal space.
If spinal stenosis develops due to arthritic debris, symptoms may become severe and may be expressed anywhere in the anatomy below the affected region of the spine. The good news related to this frightening occurrence is that arthritic change in the central canal is the type of spinal stenosis which responds best to surgical care.
At least if an operation is truly needed, it will have a good chance of succeeding. This is a rare blessing in a world filled with failed back surgery recipients.
Back Pain > Arthritis in the Spine > Degenerative Joint Disease



