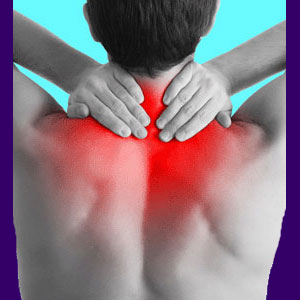
Neck injury can be a painful and slow healing ordeal which may or may not result in lasting symptoms. Cervical injuries can create pain, weakness, numbness, stiffness and tingling in the neck, shoulders and upper back.
The head acts as a weight placed on top of the neck. This weight is often a contributing factor to neck injury. When force is applied to the neck, the weight of the head will push or pull the neck beyond its normal range of movement, causing injury. This condition is commonly called whiplash.
Full coverage of a variety of symptomatic cervical conditions can be found in my neck pain section. Meanwhile, this particular essay concentrates on classifying and explaining the various possible collateral effects of trauma to the neck region.
Types of Cervical Spinal Injuries
The most common form of cervical injury is damage to the muscles and ligaments in the neck. Neck muscle pain is rarely serious, but can be horrifically agonizing while it endures.
Herniated discs are also very common in the neck. Most people demonstrate cervical disc degeneration by the time they are 30 years old. Sometimes, this degeneration can contribute to the incidence and severity of cervical disc injury.
The vertebrae in the neck are lighter and thinner than elsewhere in the spine. Combine these traits with the wide range of movement the cervical vertebrae provide and you have a good scenario for bone injury due to severe focused trauma. A fractured cervical vertebrae is commonly called a broken neck.
Treatment of Neck Injury
Most muscular injuries do not require formal treatment. Ice and heat combined with over the counter analgesics are sufficient for most soft tissue injuries.
Disc injuries may or may not cause pain. Remember that the spinal discs do not have any nerve endings and do not feel pain themselves. Pain can only be elicited when the disc influences a nearby neurological structure, such as a nerve root or the spinal cord. Even painful disc injuries usually get better within weeks, with little or no professional treatment.
Vertebral bone injuries may be more serious. Serious vertebral trauma may require require bracing or surgery to stabilize the structure. It is vital to know that just because a patient has a broken vertebrae does not mean that the spinal cord has been damaged in any way.
Spinal cord injury in the neck is very serious, since most of the bodily functions occur below the cervical levels. Complete spinal cord injury in the cervical spine can paralyze a patient from the neck down. Even minor spinal cord trauma can cause lifelong effects on motor function, autonomic function or sensory capabilities.
Guidance for Neck Injuries
Any significant neck trauma is likely to have an accompanying fear factor due to the potential for nerve damage or reduced functionality. Patients who hurt their necks must fully understand their diagnosis and receive proper support to avoid suffering a terrible nocebo effect from the diagnostic process. If psychological factors outlast the actual injury, pain may continue despite organic healing.
It is crucial to trust neck care to the most expert of medical professionals. I never recommend using any care provider who will not do everything possible to pinpoint the source of pain, including utilizing diagnostic testing, such as MRI.
I recently heard a true horror story from a patient involved in a car accident who went to a chiropractor and had a neck adjustment performed. This doctor took digital x-rays, but could not view them due to some technical glitch in their system. The chiropractor decided to do a variety of manipulations anyway. It turned out that this patient had multiple fractures and suffered cord damage and fracture migration from the adjustment. They had to be hospitalized immediately. Comparative evaluation with the x-rays taken before the adjustment showed a drastic escalation of the problems. This patient will never be the same, but is lucky to be alive and not paralyzed. Be careful out there!




