Osteoarthritis facts are important to learn as you get older and begin to demonstrate the physical characteristics of arthritis in the spine. Osteoarthritis is considered to be a degenerative condition which affects the spinal joints, although it is typically a normal and expected part of the aging process. Arthritis is not inherently painful or symptomatic, but it is one of the most common of all the back pain scapegoat conditions vilified by the medical industry. It serves this role perfectly, since it will almost always be present to take the blame for otherwise idiopathic symptoms.
This dialog provides a factual view of osteoarthritis instead of the false and often nocebo-generating profile presented to many diagnosed patients.
Understanding the Osteoarthritis Facts
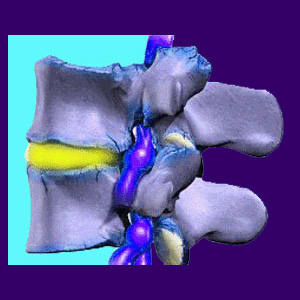
Osteoarthritis, also called degenerative joint disease or OA, is an inflammatory process which attacks the cartilage and synovial fluid in the spinal joints. These protective structures help the joint to move effortlessly and prevent bone on bone contact when the joint is put into motion. Arthritis wears away these protective measures, increasing the incidence of bone contact and the resulting osteophyte growth which often ensues.
Osteophytes, also called bone spurs, typically form in response to increased hard surface (bone on bone) contact. While osteophytes can be problematic, they can also help to reduce some osteoarthritis pain and might actually be instrumental in stabilizing affected joints.
Osteoarthritis Facts and Myths
Osteoarthritis can be uncomfortable, but is seldom responsible for widespread acute pain throughout the spine. Generally, arthritis is a normal and expected part of aging, which does not have to cause any significant symptoms in most people. Advanced or extreme arthritic changes can definitely cause severe pain and functional disability in some unlucky sufferers.
However, there are still many patients diagnosed with arthritis back pain who have been misdiagnosed, since there is no proof that their arthritic changes have enacted any pinched nerves, spinal stenosis or other painful events.
It is crucial to maintain an objective view of osteoarthritis to counter the consider nocebo effects of the diagnostic process. This is even more important to remember if your care provider frightens you with vivid worst-case-scenario descriptions of your crumbling spine. I think that many of us have received this talk, usually right before a surgical recommendation and an inquiry about what kind of major insurance we have.
Objective Arthritis Facts
Arthritis, like many other spinal conditions, can cause pain. It can create functional limitations and even warrant surgical correction in extreme circumstances. However, these are the exceptions to the rule of arthritis diagnosis.
Most patients whose pain has been blamed on OA are actually simply demonstrating completely normal and non-problematic versions of spinal arthritis appropriate for their age and activity level. In these cases, misdiagnosis is almost certain and the patient is unlikely to enjoy significant relief from any attempted back pain treatment modality.
Dorsopathy may exist, but the arthritic changes are likely to be purely coincidental to the pain or only mildly contributory. Many of these poor people are actually suffering from regional ischemia, not spinal degeneration.
If you have been diagnosed with arthritis back pain, learn the facts for yourself. If you can’t find relief, there is certainly a good chance that you, (just like many others, including myself) have been inaccurately diagnosed.



