The straight leg raising test is a common diagnostic technique mostly used in cases of suspected lumbar herniated discs. This diagnostic evaluation has been a mainstay of lower back pain treatment for decades, but is certainly a controversial practice due to many reasons. The straight leg raising test is also commonly called Lasègue’s sign, Lasègue test or Lazarević’s sign, although these names are reserved for medical personnel almost exclusively. Leg raising tests are performed by a wide range of caregivers ranging from orthopedists and neurologists to physical therapists and chiropractors.
This critical dialog explores the use of the straight leg test for lower back pain and sciatica diagnosis. We will detail the problems with the test and the reasons why most enlightened doctors now consider it to be utterly worthless in ascertaining the true cause of symptoms.
Straight Leg Raising Test Overview
The straight leg diagnostic technique is utilized in an attempt to ascertain the nature of lower back pain and sciatica complaints unilaterally or bilaterally. The test was first used in the mid 1800s and has steadily gained in popular application to this day. More and more healthcare professionals have embraced the leg raising test, since it provides a perception of “positive proof” that a herniated disc exists and therefore helps patients to acquiesce to treatment or further diagnostic evaluation, at considerable cost.
The primary idea championed by the test is that lifting a straight leg in lower back pain sufferers will often exacerbate symptoms and cause immediate agony if a herniated disc is present. It is true that most lower back pain patients do indeed suffer discomfort during this test, but not for the reasons often speculated upon. We have been speaking out publicly against the application of this test for diagnostic evaluation for many years and will use the remainder of this article to explain exactly why the test might amount to nothing more than momentary torture with no definite conclusions to be gained.
Straight Leg Raising Test Procedure
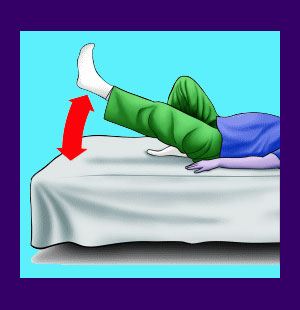
In most instances, patients are instructed to lie on an examination table on their backs in a supine position. The care provider will stand to the side of the patient or in front of them and instruct them to keep their knee straight during the test. The diagnostician will then slowly raise one leg at a time upwards and note if and when pain is expressed by the patient. Typically, the doctor or therapist will discover pain to be present between the angles of 30 and 70 degrees, although some patients suffer immediate pain and others do not suffer any exacerbation of pain, regardless of how high the leg is actually raised. In some instances, the test will be performed while the patient is seated comfortably, although this version is considered inferior by diagnosticians.
The doctor will often ask the patient to describe the nature of the pain, where it occurs and how the continuing raising affects the symptomology. Many patients find this process to be torturous and literally can’t stand the misery suffered. Doctors often take full advantage of these dramatic reactions to tell the patient that the test has indeed confirmed the presence of a herniated disc or at least suggest that an intervertebral herniation is likely to be present. Ironically, we completely disagree that the test confirms the presence of any herniated discs, (or has any diagnostic value at all) but we completely agree that a herniation is likely to be present, as explained in the section below…
Straight Leg Raising Problems
Independent research studies have shown no correlation between herniated discs and the incidence of lower back pain or sciatica. This is proven fact. These same studies have shown that lumbar herniations at L4/L5 and L5/S1 are so common that they affect more adults than not in some age demographics.
Straight leg raising is supposed to demonstrate that one or more lumbar nerve roots are affected, causing the painful expression when the spinal canal constricts. However, there are many possible reasons for these nerve roots to suffer compression and herniated discs are just one of them. Other problems affecting these nerve roots might also be exacerbated by leg lifting, since the lumbar spinal canal is constricted during the test and the foraminal openings are narrowed at the base of the spine.
The test does not take into account that the majority of sciatica complaints are not caused by spinal origins, but instead are induced by structural soft tissue problems or nonstructural ischemia concerns. Ischemia is also a common causation of all varieties of chronic back pain is statistically affects the lower back more than any other anatomical target. Raising a straight leg will cause pain in most soft tissue and nonspinal joint conditions, including sacroiliac, hip and muscular pain syndromes. These facts are rarely considered by spinal-focused diagnosticians during the leg raising test.
Straight Leg Raising Test Experiences
I have endured this ridiculous test on many occasions over decades of time in the back pain treatment sector. I always tell doctors ahead of time that the test will hurt me and even tell them that I have virtually no flexibility left when my leg is straight. They seem to disregard the information and proceed anyway, some even seeming to enjoy the grimacing on my face as I stop them from proceeding any higher due to overwhelming agony. It is all a bit sadistic in my opinion. I do have multiple herniated discs in my lower back, as well as throughout my spine, but these discs have not been definitively implicated in causing my pain when evaluated by objective quality care providers.
Similarly, many patients have written complaining of the torture that they have endured by doctors and chiropractors during this test. Some have cited worsened symptomology for months or even years following the test. Meanwhile, nothing is ever gained in the diagnostic process from performing the exam.
I suggest that if and when the test is ever used, it is performed cautiously and with respect for the likelihood of generating potentially severe pain. It would be better if the test were simply skipped over and diagnostic imaging performed, since this is a far superior way to ascertain the true underlying causative factors of most structurally-induced pain syndromes. Additionally, I would also love to see more emphasis on diagnostic evaluation of nonstructural pain mechanisms, such as the aforementioned oxygen deprivation syndromes that are a literal epidemic in the modern healthcare industry.




