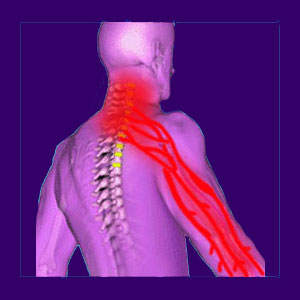
A weak arm is one of the usual complaints of patients who suffer with a wide range of upper back pain and neck pain conditions. Weakness in one or both arms can result from a great number of reasons and does not necessarily indicate neurological involvement in the spine. Weakness can be scary, especially when it comes on suddenly and to a significant degree. Remember that any acute arm symptoms should be reported to your doctor immediately, since they might indicate a potentially serious medical problem, such as a heart attack.
Arm weakness is often used to justify treatment of the upper vertebral column, even without definitive evidence that the symptom is related to the suspected spinal source. It is for this reason that we provide this report in order to help patients to better understand the nature of their symptoms and avoid the common incidence of misdiagnosis that is so common with various types of neurological expressions. This guide details weakness in one or both arms, including the potential causes of the issue and the symptomatic signs that each particular causation creates.
Weak Arm Factsheet
Verifiable weakness is also called objective weakness. This is not the feeling of being weak, but instead it is the actual diminution of the muscles’ ability to function normally. This type of weakness can be diagnosed using specialized neurological tests. When objective weakness is discovered, the chances for spinal structural causation increase, but there are still other potential causes that can create identical results.
Far more common is the experience of subjective weakness, or the perceived feeling of being weak. The muscles demonstrating this type of weakness often check out just fine during diagnostic testing and this fact helps eliminate many possible sources of symptoms in the spinal anatomy.
In order to best classify which type of weakness is presented, it is advised to seek evaluation from a spinal neurologist. These doctors are ideally qualified to perform the type of diagnostic processing that all neurological expressions justly deserve.
Weak Arm Causes
There are many possible spinal, nonspinal and nonstructural causes of arm weakness detailed in the section below:
Cervical spinal stenosis can cause weakness in the arms in rare instances. Far more common are symptoms in the legs, but this is not an absolute rule.
A pinched nerve root in the neck or upper back is a common cause of weakness in one arm. Typically, this scenario will begin as localized pain in the area of compression and tingling in the affected area of the arm. The symptoms will progress to numbness and then weakness in the affected arm musculature. This diagnosis is often unenlightened and found to be incorrect, since true nerve compression will create objective weakness, but not subjective weakness. Remember that the majority of patients suffer perceive weakness rather than actual diminished ability.
Thoracic outlet syndrome can also create a weak feeling in the arms and may actually enact objective numbness and weakness together, due to neurological involvement or circulatory issues.
Weakness in the arm might also be a result of localized nerve or muscle damage in the shoulder or arm itself. Usually this is caused by an obvious event and should not pose diagnostic challenges for this reason. Shoulder weakness might be more prevalent than arm weakness.
Systemic processes, such as neuromuscular diseases and diabetes, might also be responsible for weakness in one or both arms. However, symptoms will likely affect other areas of the body, as well, and should be easily diagnosed through basic testing and evaluation of the patient’s general health.
Mindbody-enacted ischemia can affect the spinal nerve roots or localized nerve and muscle tissues in the exact same manner as structural compression or injury. Oxygen deprivation can cause all manner of symptoms and dysfunctions, including weakness in the arms.
Arm Weakness Treatment Cautions
In all cases, treatment of arm weakness should be delayed until a verified diagnosis is ascertained. Premature treatment of symptoms usually produces poor outcomes and might result in catastrophic consequences to general health, especially in cases of pharmacological pain management or minimally invasive surgeries. Remember that treatments have little hope for efficacy if they are not targeting the actual symptomatic source.
Many, many weak arm conditions are blamed on coincidental spinal irregularities in the cervical region, usually implicated as causing nerve compression. A talented diagnostician would discount many of these scenarios, since there is often a lack of correlation between the actual and expected symptoms in terms of location or breadth. Basically, there is no evidence of neurological compression and the symptoms do not even match what should happen if the suspected nerve was compressed.
Countless people undergo surgery for such unverified compressive neuropathy conditions each year, mostly enduring poor outcomes. To avoid this fate, remember that bulging discs, osteoarthritis, spinal stenosis and foraminal stenosis are all normal occurrences in the vertebral levels that innervate the arms. In only a few circumstances do these conditions generate symptoms, but in many cases are they unfairly blamed for being pathological. Be sure to seek out a second or third opinion on any spinal nerve root compression diagnosis before considering any type of moderate or drastic care.




