The diagnosis of herniated discs can be a scary experience for any patient. We have all heard horror stories about disc injuries and how some patients never recover. Therefore, this diagnosis can create a powerful nocebo effect on the patient that can last forever. Many patients never get past the idea that a structure in their back has failed and now they perceive themselves to be permanently damaged goods.
The scope of this article will look at the actual diagnostic process used to identify disc protrusions in the human spine. However, the psychological effects of herniations will also be discussed, since these are just as important to understand as their physical counterparts.
Diagnosis of Herniated Discs Methods
Diagnosing a herniated disc is usually accomplished by a medical doctor or chiropractor. The diagnosis is typically made through a series of progressive steps:
First, the care provider will interview the patient about the nature of their pain and their general health. Any instances of back or neck injury should be thoroughly discussed and evaluated.
A physical exam should always be performed to check for pain, tingling, numbness or weakness anywhere in the anatomy.
X-rays might be performed, but they will not show a herniated disc. They may however, provide enough evidence of a potential disc abnormality to order an MRI study.
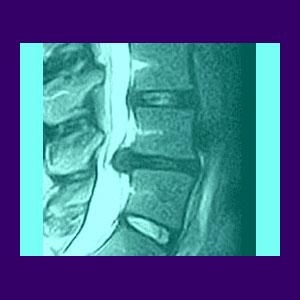
MRI of the spine can confirm almost any variety of disc injury. MRI can also visualize many of the soft tissues which may contribute to a symptomatic expression, such as ligamentum flavum hypertrophy.
CT scan, also called computed tomography, is less expensive than MRI and can also effectively diagnose many disc issues. CT is not as useful for determining possible neurological effects of said herniation, however.
Myelogram is an advanced test to detect disc abnormalities and other spinal problems.
Mindbody Effects of Herniated Disc Diagnosis
As previously mentioned, the diagnostic pronouncement of a disc pathology is always psychologically damaging. This is true whether the diagnosis is herniation, degeneration, bulge or rupture. Patients often report suffering a severe escalation of symptoms shortly after diagnosis of a herniated disc and this can easily be explained by the nocebo effect. The way to fight the negative psychoemotional consequences of the diagnostic process is with the simple power of knowledge. Patients fear what they do not know or understand.
Patients also fear the misconceptions and myths they have been told all their lives about herniations. Learning the facts about disc conditions will set them free from this considerable worry and anxiety. The diagnostician should always consider the psychological factors and must do everything in their power to tell the patient the simple truths of herniated discs and how most are nothing of concern.
Unfortunately, many opportunistic doctors take the opposite stance, purposefully vilifying even the most innocent disc abnormalities in order to profit financially from extended or drastic treatment. In my 25 years active research and participation in the back pain treatment sector, I see this all the time, but it still sickens me at each and every occurrence.
Beware the Inaccurate Diagnosis of Herniated Discs
Beware of chiropractors, or other care providers, who say they can diagnose herniated discs by a simple physical exam. There is no sure way to determine a disc injury through touch or clinical exam. Personally I have met at least a few chiropractors who insisted they can feel even slight disc irregularities with their touch alone. No, the straight leg raising test means absolutely nothing and does not correlate to the incidence of disc herniation. This is an antiquated myth at best and a purposeful deceit at worst. If you are being treated by an care provider who claims to have a “magical” ability to diagnose by sight or touch alone… run. Run quickly and don’t look back.
An MRI is always a safe bet when a herniated disc is suspected. This will confirm the existence of a herniation, as well as show any potential neurological effects the disc might be creating in the spine.




