Facet joint back pain is a very common diagnosis which typically turns out to be incorrect or only partially correct in many cases. Facet syndrome remains a very controversial diagnostic theory among doctors, since many of the physical characteristics are considered to be normal parts of spinal aging, rather than pathological developments.
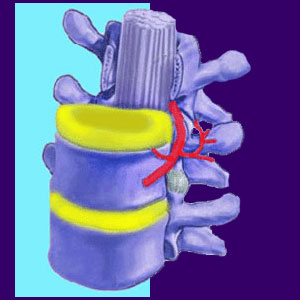
The facet joints are the interesting looking fin-like projections on the rear of most vertebrae. These joints help support and stabilize the vertebral bones as they move against each other in the full range of motion available to humans. In the case of facet joint syndrome, these very structures are blamed for enacting symptoms, typically due to either injury, or more commonly, spinal degeneration.
This essay examines the role of facet hypertrophy in the expression of a variety of acute and chronic back pain symptoms.
Causes of Facet Syndrome Back Pain
There are 2 main sources of diagnosed facet joint pain:
The first source is traumatic injury and this theory often turns out to be correct, especially for acute, short-term dorsopathy complaints. The facet joints can fracture or break, like any bone, and this can cause severe pain, especially upon movement of the affected vertebral level.
The usual diagnostic theory of facet syndrome does not involve injury, but is instead blamed on the normal and universal degenerative processes involved in spinal aging. Spinal arthritis causes the break down of the synovial structures in the facet joints, creating added friction and contact between the bones.
Osteophytes, also called bone spurs, build up around the facet joints and are the main suspected culprits in most pain syndromes. In some cases, this theory is correct, but in most, the occurrence of arthritis is coincidental to any symptoms endured. No definitive link exists between the presence of spinal degeneration and the incidence of back or neck pain.
Facet Joint Pain Diagnosis
Facet joint syndrome is rarely the first diagnostic theory employed by doctors. However, barring any major disc issues or other structural concerns, facet joint degeneration, which can be clearly imaged with MRI technology and at least seen to some degree on x-rays, may become a major player in the suspect pool.
True facet joint pain is rather distinctive in most cases, being linked to specific movements and providing dull and achy sensations, rather than the sharp and chronic symptoms of most other typical dorsopathy complaints.
Symptoms should exist locally in a well defined area, not move about or occupy large regions of the back. Symptoms should definitely not be experienced far off center of the spine itself, as is often the case.
Facet Joint Back Pain Guidance
Blaming normal facet joint degeneration for enacting chronic and severe back pain is generally as unenlightened as blaming a mild herniated disc or degenerative disc disease for sourcing significant symptoms. This is especially true for cases not involving traumatic back injury or extreme arthritic change. In many patients, the diagnosis is made simply because no other structural reason exists and subsequent treatment will provide monetary incentive for the doctor to pronounce some cause for the symptoms to exist.
The good news is that most correctly diagnosed facet syndrome conditions respond very well to indicated treatment options. However, if your facet joint pain has not improved despite a variety of therapy options, you must seriously consider the validity of the diagnostic theory, or else risk being in pain for life.



