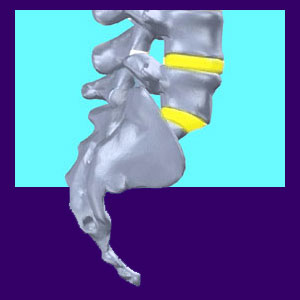
Facet joint degeneration is a general term used to describe the condition which is commonly diagnosed as facet joint syndrome or facet joint disease. The facet joints are often areas of arthritic activity, since they get a tremendous amount of wear and tear, particularly in the neck and lower back regions.
Although facet degeneration is normal and universal, it is sometimes used to explain back pain symptoms and in some cases, this diagnosis may be correct. However, in the overwhelming majority of diagnosed patients, facet disease is not a disease at all and demonstrates an extremely low probability of being the true source of the painful expression.
This treatise explores the degenerative processes that work on the spinal facet joints and their common effects on vertebral form and function.
Facet Joint Degeneration Definition
The facet joints link the posterior of each vertebral body together from superior articular process to inferior articular process. These joints help provide support for the spinal column and incredible flexibility and stability of movement.
The facet joints are synovial joints, which mean that they contain areas of cartilage surrounding small fluid filled sacs which help to lubricate joint movement and prevent bone on bone contact. However, as we age, it is normal and expected for these protective mechanisms to break down in the facet joints and in most major joints in the body. This leads to the incidence of osteoarthritis, which is also virtually universal, particularly in the cervical and lumbar spinal zones.
Facet Degeneration Symptoms
The physical indications of facet syndrome include a noticeable decrease in cartilage and the loss of synovial fluid from the joints. This is followed by the wearing away of the bone surface and possible formation of osteophytes, also commonly known as bone spurs, on or around the facet joints. While this process sounds quite fearsome, it is mostly innocent and asymptomatic, and most people never even know it is occurring.
In some cases, facet degeneration can become problematic, especially when the arthritic change is extreme at a particular level. Bone spurs are the usual culprit when symptoms do exist and may enact pain from bone on bone contact, although this typically involves a specific range of motion and may resolve over time as the spur naturally grinds down.
Bone spurs can also enact nerve compression if the osteophyte forms in or around the neuroforaminal space, although many pinched nerves turn out to be clearly misdiagnosed when correlated clinically.
Diagnosis of facet degeneration as the source of pain is often a process of elimination, utilizing less than precise methods, such as anesthetic injections. While doctors call this diagnostic processing, I call it guessing.
Facet Joint Degeneration Factsheet
The reason I see little evidence which supports facet degeneration as the actual source of pain in most diagnosed patients is actually twofold.
First, the surgical treatments used during treatment actually change the anatomy and should relieve the pain, but rarely do. Meanwhile, non-traditional approaches, like knowledge therapy, can work wonders for patients despite the structural degeneration remaining.
Second, the symptoms expressed usually do not correlate to the diagnosed source. Facet joint pain involves mechanical interactions or tiny neurological structures which will create pain locally. Many patients have widespread regional pain. This is illogical.
It is crucial to remember that facet joint disease is truly something which affects all of us. However, most of us never know it and never care, since there is no pain. When back pain does exist, it may, in rare circumstances be correctly linked to the anatomical changes, but in most patients will be coincidental to the structural issues. This goes for many of the typical dorsopathy scapegoats and is certainly not limited to facet syndrome.




