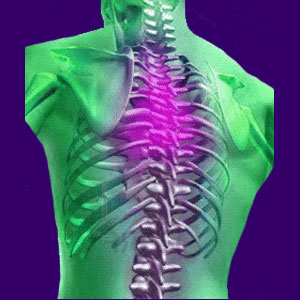
Thoracic outlet pain can express itself in between the shoulders, in the entire upper back, in the lower neck or even in the upper appendages, depending on the circumstances of the causative process.
Thoracic outlet syndrome is a growing diagnosis in the medical sector and can be the result of neurological or vascular compression enacted by back injury or idiopathic reasons, including nonstructurally-motivated regional oxygen deprivation. Pain is most often accompanied by neurological expressions, as well, including pins and needles and paresthesia in affected locations. Sometimes, when vascular compression occurs, the sure signs of structural ischemia will be present including changes in skin and possibly the experience of complete numbness.
This dialog investigates TOS pain syndromes and profiles the many variables inherent to the diagnosis of thoracic outlet conditions.
Types of Thoracic Pain
Thoracic outlet syndrome symptoms take many forms, depending on the nature of the cause and the severity and duration of the muscular compression. Most patients experience severe pain in between the shoulder blades and experience difficulty in utilizing the arms. Some patients suffer pain in the neck and base of the skull and may have a difficult time moving the head comfortably. Still others have the majority of their pain in one or both shoulders, arms or hands.
Pain may be constant or linked to position or activity level. Symptoms may be generalized throughout the upper back and neck or may emanate from a specific area of the back. Pain may be steady or come in waves or spasms. Upper back spasms associated with TOS can be very severe and may force the patient into bed until the attack passes.
Thoracic Outlet Pain Mechanisms
TOS is characterized by symptoms which are enacted in the brachial plexus. This upper back nerve center can be affected by injury, just like any other area of the spine. Typically, injuries to the upper back muscles may cause inflammation, leading to muscular interaction with the brachial nerve structures. The most common tissues implicated in these occurrences are the scalene muscles.
TOS can also come from ischemia of the area, either due to physical compression or mindbody oxygen deprivation. Ischemia of the nerve structures in the brachial plexus can be agonizing and may last until the underlying causative source is discovered and successfully treated.
Usually in structural cases, this blood restriction is enacted by constriction of the subclavian vein and/or artery by the scalene muscles. In nonstructural cases, the process is usually enacted by the subconscious mind as a defense mechanism against emotional life-stressors.
Thoracic Outlet Painful Symptoms
Thoracic outlet syndrome may certainly be the result of actual structural damage or genetic predisposition due to an unusual muscular anatomy. Injuries which enact TOS pain typically resolve in a matter of days or weeks, even without any formalized medical care. People with a genetic predisposition to muscular involvement with the brachial nerves may have the ideal circumstances for chronic or recurrent thoracic outlet syndrome episodes. These are the patients who statistically benefit most from drastic and possibly surgical methods of care.
Some diagnosed patients will be suffering from some form of ischemia of the upper back tissues. Once again, when the muscles are truly responsible, treatments will generally provide lasting resolution of the restricted blood flow. Patients who are suffering from mindbody oxygen deprivation may find successful treatment using knowledge therapy. Like many other structural-based diagnoses, doctors typically only see the results of oxygen deprivation, but ignore the possible underlying psychoemotional roots of the condition. It is for this reason that patients who suspect a possible link to emotional contributors should investigate the possibility of a nonstructural causation.




