There are several possible causes of thoracic outlet syndrome, although some of these theories might be completely misidentified as the actual reason for the painful complaint in many diagnosed patients. It is so important to achieve an accurate diagnosis for your TOS symptoms, just like for any other back pain syndrome. Unfortunately, finding out the real reasons for your pain might prove more of a challenge than it first appears to be. This is why so many patients suffer disappointing results from their attempts at treatment.
This detailed essay provides coverage of the many possible causes of both true thoracic outlet syndrome, as well as symptoms that might mimic TOS, but are actually not created from structural brachial plexus compression.
Structural Causes of Thoracic Outlet Syndrome
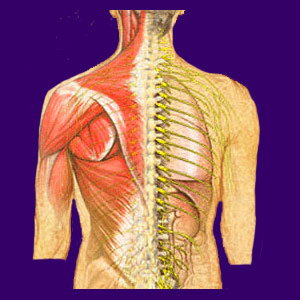
Most cases of thoracic outlet syndrome are theorized to be created due to anatomical compression of one or more components of the brachial plexus. This is a cluster of neurological tissue which exists in the upper back, providing nerve function for much of the torso and arms. Some TOS conditions are blamed on compression of the subclavian vein or subclavian artery. This compression might be linked to movement of a skeletal structure or muscular structure (such as the shoulder) against these tissues. Thoracic outlet might also be theorized to exist due to constant general muscular compression of the regional area, generally involving the scalene muscles of the upper back.
Diagnostic theories in particular patients often change and evolve as testing implicates or exonerates particular structures as being part of the overall symptomatic process.
Mindbody Causes of Thoracic Outlet Pain
While it is possible to experience neurological, arterial or venous compression from some anatomical structure in the upper back, these events are rare. Far more common is the incidence of simple ischemia enacting TOS type symptoms in the nerves of the brachial plexus and even in the muscles of the upper back and neck. This type of pain is typically misdiagnosed and becomes stubbornly persistent, since therapies are not targeting the actual source of pain. This certainly helps to explain why so many back pain patients with thoracic outlet syndrome never fully recover.
To resolve this type of oxygen deprivation pain, the suffering person must pass by the traditional medical back pain treatments and give up the complementary medical therapies they have relied upon unsuccessfully. The answer for any psychosomatic pain syndrome is knowledge therapy, since this treatment is the only one which addresses the underlying emotional issues at the heart of the symptom imperative.
Causes of Thoracic Outlet Syndrome Exploration
Many people who perform repetitive motions with their arms or hands are at a higher risk for developing TOS. Additionally, people who sit and type for long periods of time are at equal risk. Many serious athletes, such as swimmers and ball players are diagnosed with TOS, as well.
Many of these people are actually suffering from the anatomical demands they have placed on their bodies, but a few have fallen victim to the ever-increasing incidence of diagnosis of this pain condition and the nocebo reaction the diagnostic method provides. This fact is even more true for people who have not suffered a serious upper back injury.
For patients with chronic unresponsive TOS, there may be other more logical explanations for the symptoms which should be considered. Regional ischemia is surely one to explore. However, some patients might demonstrate yet undiagnosed cervical spinal issues which may mimic the symptoms of TOS exactly. This is why it is always wise to see your neurologist about any speculative nerve pain condition and be sure to undergo diagnostic testing which can definitively confirm the theoretical cause before seeking treatment.
Back Pain > Thoracic Outlet Syndrome > Causes of Thoracic Outlet Syndrome




